Women’s health is complex, and many common female health issues go unrecognized or untreated for years. Hormonal shifts, reproductive concerns, and mental health challenges often intersect in ways that affect your daily life.
At Mosaic Medicine Clinic, we believe every woman deserves clear information about what’s happening in her body. This guide covers the health issues you should know about and when to reach out for support.
Hormonal Imbalances and What They Actually Mean
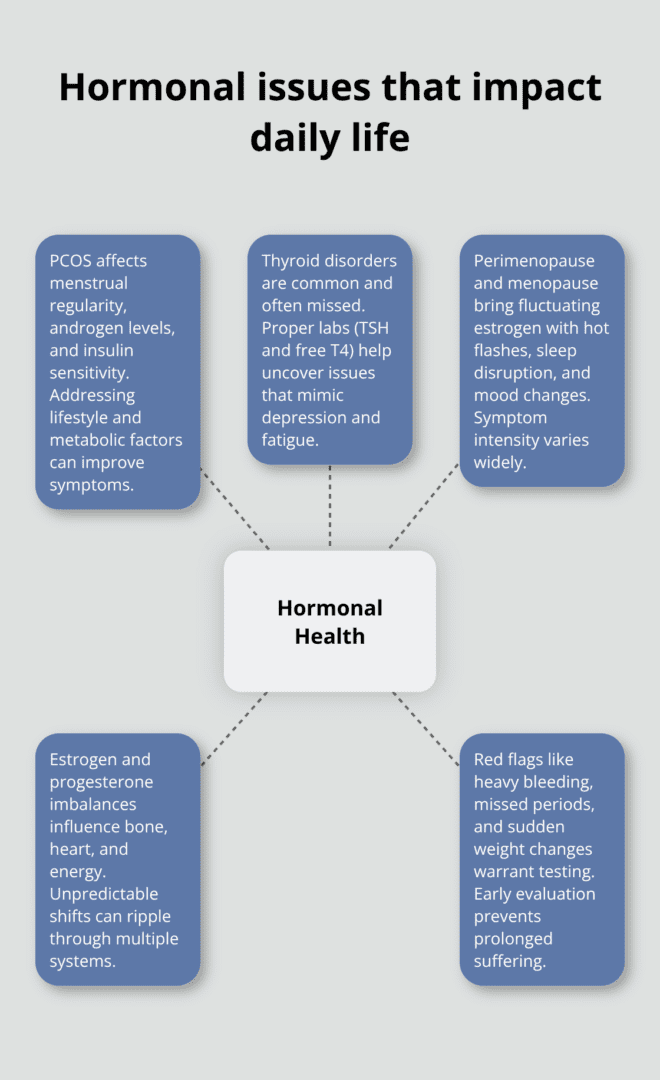
Your hormones control far more than your mood. Estrogen and progesterone fluctuations drive your menstrual cycle, bone density, heart health, and energy levels. When these hormones shift unpredictably, the effects ripple through your entire body.
PCOS: A Common Diagnosis That Responds to Action
PCOS affects roughly 1 in 10 women of reproductive age according to the CDC, and it presents with irregular periods, excess androgen levels, and insulin resistance. If you have PCOS, lifestyle changes matter significantly. A 2019 study published in Nutrients found that women with PCOS who followed a low-glycemic diet and completed regular exercise saw improvements in insulin sensitivity and menstrual regularity within 12 weeks.
Thyroid Disorders: Often Missed, Always Treatable
Thyroid disorders are equally common but frequently missed. About 1 in 8 women will develop a thyroid condition in her lifetime according to the American Thyroid Association. Hypothyroidism causes fatigue, weight gain, and depression that feel like personal failings when they’re actually a medical issue requiring treatment. Ask your provider for TSH and free T4 testing, not just a basic TSH screening, because some thyroid problems hide in normal-range results.
Menopause and Perimenopause: Expect the Unexpected
Menopause typically arrives between ages 45 and 55, but perimenopause can start a decade earlier. During this transition, your estrogen drops unpredictably, triggering hot flashes, night sweats, sleep disruption, and mood changes that last months or years. The intensity varies wildly between women, and that variation is normal.
Red Flags That Demand Evaluation
Severe menstrual bleeding that soaks through multiple pads or tampons in an hour, periods lasting longer than seven days, or bleeding between cycles all warrant medical attention. Heavy bleeding causes iron deficiency anemia, which worsens fatigue and brain fog. Missed periods for three months or longer, even if you’re not pregnant, signals a hormonal problem needing investigation.
Sudden weight gain of 10 pounds or more without dietary changes points toward thyroid dysfunction or PCOS. Severe mood swings, depression, or anxiety that worsen at specific points in your cycle deserve evaluation because hormonal fluctuations genuinely affect mental health. Extreme fatigue that rest doesn’t fix, hair loss, or skin changes also warrant testing.
Schedule an appointment with a primary care provider or gynecologist who orders appropriate bloodwork. Don’t accept dismissal of your symptoms as stress or age-related without testing. Getting the right diagnosis changes everything about your treatment approach, which is why thorough hormone evaluation matters so much. Your reproductive health concerns-from irregular periods to fertility questions-often connect directly to these hormonal patterns, and addressing them early sets the foundation for better outcomes.
Reproductive Health Concerns
Endometriosis and Fibroids: Two Different Problems, Similar Symptoms
Endometriosis and uterine fibroids produce remarkably similar symptoms, which causes many women to treat the wrong problem for years. Endometriosis is when tissue that is similar to uterine tissue grows someplace else. It can cause pain, irregular periods and infertility. Fibroids are benign tumors that develop within or on the uterine wall. Both conditions cause severe pelvic pain, heavy menstrual bleeding, and fertility problems, yet they require completely different treatment approaches.
The distinction matters enormously because the diagnostic process differs. A surgeon must perform laparoscopy to confirm endometriosis-a procedure where they view your pelvic organs directly. Fibroids show up on ultrasound or MRI without surgery. Treatment approaches diverge sharply: hormonal therapy works for endometriosis management, while fibroids sometimes need myomectomy surgery to remove individual tumors or, in severe cases, hysterectomy.

If you experience debilitating period pain that keeps you from work or school, bleeding so heavy you change protection every hour, or pain during intercourse, push for imaging and specialist referral rather than accepting pain as normal. Many women suffer for a decade before getting proper diagnosis because these conditions aren’t automatically suspected during routine visits.
Irregular Periods and Fertility: Track Your Patterns
Irregular periods and fertility struggles frequently trace back to hormonal imbalances you can actually address. When your cycle shifts from predictable to chaotic, or when you’ve been trying to conceive without success for over a year, thyroid function and insulin resistance deserve investigation before assuming infertility requires expensive interventions.
Track your cycle length, flow intensity, and any spotting between periods for three months and bring this data to your appointment. Patterns reveal underlying problems that bloodwork alone might miss. This simple tracking habit gives your provider concrete information to work with during evaluation.
Screening That Prevents Serious Disease
Preventative screening protects you from serious conditions hiding behind common symptoms. Abnormal vaginal bleeding after intercourse, between periods, or after menopause warrants evaluation because it can signal endometriosis, fibroids, polyps, or cancer.
Pap tests starting at age 21 catch precancerous cervical changes before they become dangerous. HPV testing identifies high-risk infection types 16 and 18 that cause cervical cancer. The American Cancer Society recommends Pap screening every three years through age 65, or HPV testing every five years if that’s your clinic’s protocol.
Regular gynecologic exams matter because your provider can detect fibroids, assess pelvic floor function, and spot early warning signs during physical examination. Early detection genuinely changes outcomes. Precancerous cervical cells respond beautifully to LEEP procedure, a simple office treatment that removes abnormal tissue and prevents cancer development. Women who skip screening face much higher cervical cancer risk, yet this cancer is largely preventable with routine care.
Your mental health and emotional wellbeing connect directly to these reproductive health challenges, which is why addressing both physical symptoms and psychological impact matters for your overall recovery and quality of life.
Mental Health and Hormonal Health Are Inseparable
Your hormones shape your mental health in ways that standard mental health treatment often misses entirely. Depression and anxiety spike during specific phases of your menstrual cycle for a biological reason, not a personality flaw. Research from the NIH shows that women experience depression at roughly twice the rate of men, and hormonal fluctuations account for a significant portion of this difference. If you notice your anxiety intensifies right before your period or your mood crashes during ovulation, that’s not coincidence. The estrogen drop before menstruation alters serotonin availability in your brain.
Many women receive antidepressant prescriptions for symptoms that actually stem from unmanaged hormonal fluctuations, which means they’re treating the wrong problem. Track your mood alongside your cycle for two months. Write down when you feel most anxious, when depression hits hardest, and when you sleep poorly. Bring this information to your appointment because it guides whether you need hormonal intervention, mental health support, or both.

Some women find that addressing PCOS or thyroid dysfunction dramatically improves their anxiety without additional psychiatric medication. Others need antidepressants plus hormone management. The key is getting evaluated by someone who understands the connection rather than treating mental health and reproductive health as completely separate issues.
Sleep Disruption Demands Real Solutions
Sleep disruption during perimenopause and menopause destroys your quality of life in ways that go far beyond feeling tired. Changes in sleep patterns can happen during this time, triggering a cascade of problems: impaired cognitive function, worsening mood, increased inflammation, and weakened immune response. You cannot think clearly, manage stress, or maintain emotional stability when you’re sleep deprived.
Stop accepting this as inevitable. Cognitive behavioral therapy for insomnia (CBT-I) shows genuine results-the NIH reports it works as effectively as sleep medication for many women. Cool your bedroom to 65 to 68 degrees Fahrenheit, use moisture-wicking bedding, and wear breathable sleepwear. Limit caffeine after 2 PM because it disrupts sleep architecture even if you don’t feel jittery.
Exercise helps tremendously-try 150 minutes of moderate activity weekly to improve sleep quality-but avoid intense workouts within three hours of bedtime.
Your Support System Changes Everything
Your support system during hormonal transitions matters more than you might think. Women who feel isolated or unsupported during perimenopause and menopause report significantly worse symptom severity and longer recovery periods. This isn’t weakness; it’s biology.
Talking with other women experiencing similar changes normalizes what feels like losing your mind. Online communities, support groups, or conversations with friends navigating the same transition provide validation that your symptoms are real and manageable. A trusted healthcare provider who listens without dismissing your concerns becomes your partner in this transition rather than another person minimizing your experience.
Final Thoughts
The common female health issues covered in this guide-hormonal imbalances, reproductive concerns, and mental health challenges-rarely exist in isolation. They overlap, influence each other, and demand attention before they compound into serious problems. Your body sends signals constantly, and learning to recognize them changes your health trajectory.
Preventative care catches problems early when treatment works better and costs less. Regular checkups with a provider who listens establish a baseline for what’s normal for your body, making it easier to spot when something shifts. Pap tests, blood pressure checks, thyroid screening, and bone density assessments form the foundation of staying healthy.
Taking control of your health journey means refusing to accept dismissal of your symptoms and finding a healthcare partner who treats you as an expert on your own body. We at Mosaic Medicine Clinic believe you deserve unrushed appointments with a doctor who actually listens, which is why our membership-based approach provides direct access to your physician and time to discuss what matters most to your health. Connect with us at Mosaic Medicine Clinic in Bradenton, Florida to start your health journey with a partner genuinely invested in your wellbeing.