Women’s sexual desire fluctuates throughout their lives, and hormones influence these changes in powerful ways. Estrogen, testosterone, and other hormones directly impact libido, arousal, and overall sexual satisfaction.
At Mosaic Medicine Clinic, we see many women struggling with hormone-related changes to their sexual health. Understanding how hormones and female libido connect helps women take control of their intimate wellness and find effective solutions.
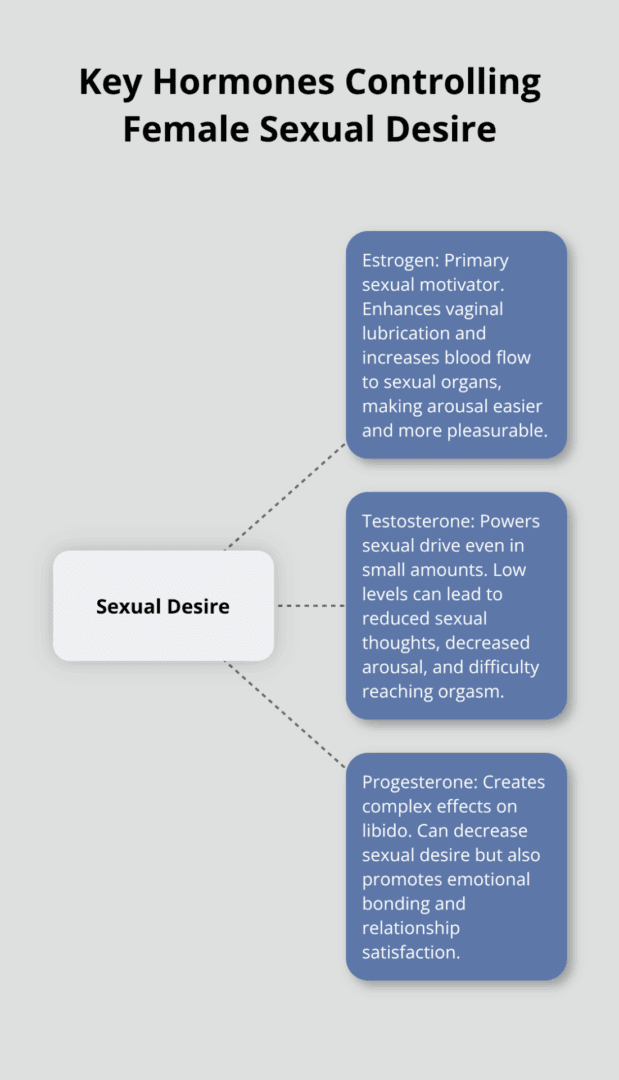
How Do Three Key Hormones Control Your Sexual Desire?
Three hormones work together to control women’s sexual desire, and understanding their specific roles helps you identify why your libido changes throughout your cycle.
Estrogen Acts as Your Primary Sexual Motivator
Estrogen drives sexual motivation and arousal in women. Estrogen-only therapies that produce periovulatory levels of circulating estradiol increase sexual desire in postmenopausal women. This hormone enhances vaginal lubrication and increases blood flow to sexual organs, which makes physical arousal easier and more pleasurable.
Women typically experience peak sexual desire mid-cycle when estrogen levels reach their highest point (around day 14 of a 28-day cycle). Studies document that up to 26% of surgically postmenopausal women experience persistent lack of sexual desire, highlighting estrogen’s critical role in maintaining libido.
Testosterone Powers Sexual Drive Even in Small Amounts
Testosterone influences women’s sexual desire despite existing in much lower levels than in men. Studies by Davis and team demonstrate that testosterone at supraphysiological levels enhances the effectiveness of low-dose estrogen therapies for increasing sexual desire.
Women produce testosterone in their ovaries and adrenal glands, with levels naturally declining after age 30. Low testosterone often manifests as reduced sexual thoughts, decreased arousal, and difficulty reaching orgasm. However, physiological doses of testosterone alone show no significant increase in sexual desire according to research findings.
Progesterone Creates Complex Effects on Libido
Progesterone produces mixed effects on sexual interest throughout your cycle. Levels rise after ovulation and during pregnancy, often leading to decreased sexual desire in many women. The luteal phase, when progesterone dominates, frequently correlates with reduced libido and increased fatigue.
However, progesterone also promotes emotional bonding and relationship satisfaction, which can indirectly support sexual connection. Women using progesterone-based contraceptives often report changes in sexual desire patterns compared to their natural cycles.
These hormonal fluctuations create predictable patterns that change dramatically throughout different life stages, from your monthly cycle to major transitions like pregnancy and menopause.
How Does Your Libido Change Through Major Life Stages?
Your Monthly Cycle Creates Predictable Desire Patterns
Women experience distinct libido patterns during their 28-day menstrual cycle, with sexual desire reaching its peak around day 14 when estrogen hits its highest levels. Research by Stanislaw and Rice shows a significant mid-cycle increase in women’s self-reported sexual desire, which correlates directly with hormonal fluctuations.
The follicular phase (days 1-14) brings gradually increased sexual interest as estrogen levels rise, while the luteal phase (days 15-28) often delivers decreased desire as progesterone takes control. Women who track their cycles report their strongest sexual urges 2-3 days before ovulation, when testosterone also peaks slightly.

This pattern becomes less predictable for women who use hormonal contraceptives, which suppress natural hormone fluctuations. A systematic review of 36 studies involving more than 13,000 women reported no significant changes in sexual desire with the use of oral combined contraceptives.
Pregnancy and Postpartum Bring Dramatic Hormonal Shifts
Pregnancy creates massive hormonal changes that affect sexual desire in waves. First trimester fatigue and nausea typically reduce libido, while the second trimester often brings increased sexual interest as blood flow to pelvic organs increases. Third trimester physical discomfort usually decreases desire again.
Postpartum recovery involves plummeting estrogen levels, especially during breastfeeding, which can suppress sexual desire for 6-12 months. Women who breastfeed produce high prolactin levels that actively inhibit sexual interest-an evolutionary mechanism to space pregnancies.
Many women don’t return to pre-pregnancy libido levels until after they wean, when hormones gradually normalize.
Menopause Permanently Alters Sexual Desire Landscape
Menopause occurs at an average age of 52 in the United States and brings permanent changes to sexual desire through declining estrogen production. Up to 26% of postmenopausal women experience persistent lack of sexual desire according to Leiblum’s research.
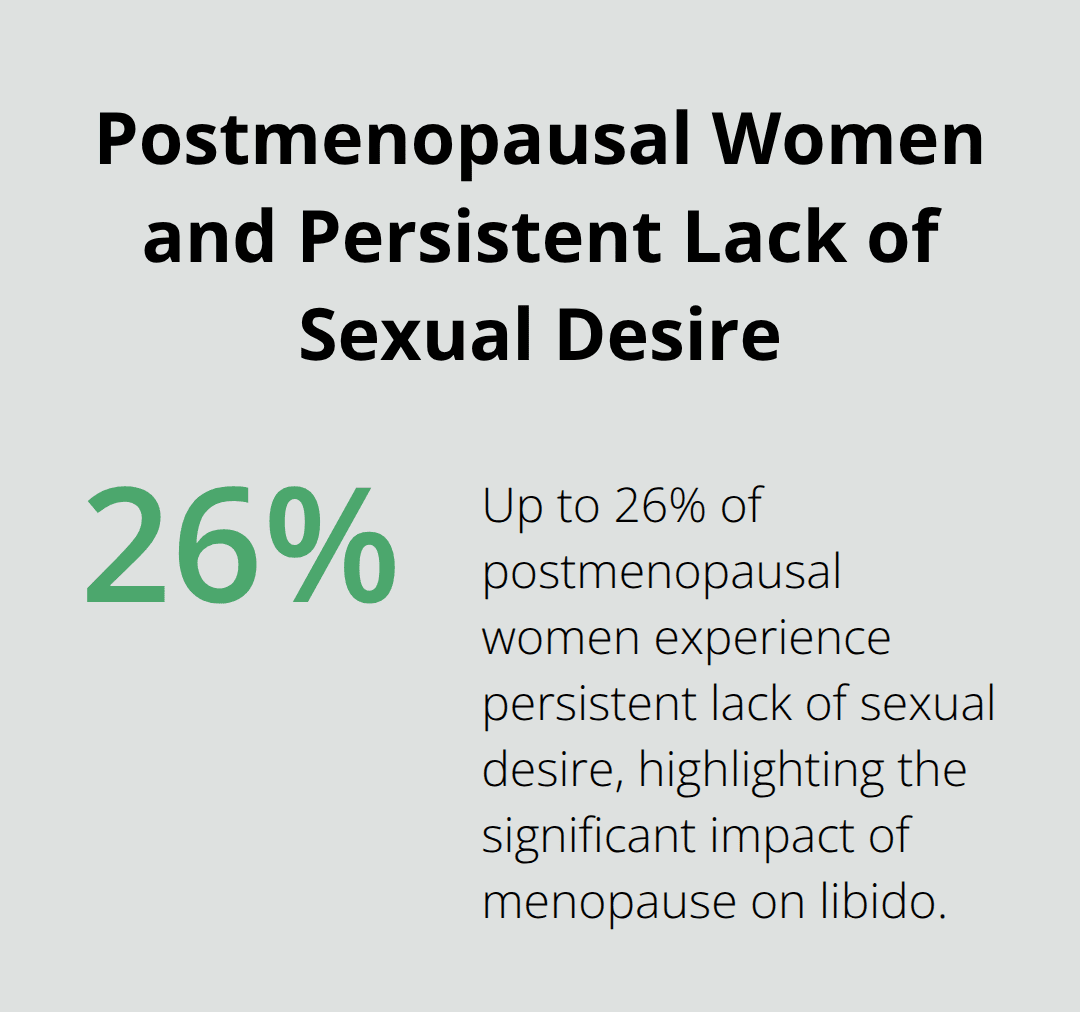
Perimenopause symptoms like hot flashes, irregular periods, and mood changes often begin 4-10 years before menopause and gradually reduce sexual interest. Post-menopause decreased estrogen causes vaginal dryness, reduced blood flow to sexual organs, and thinning vaginal tissues that make intercourse uncomfortable.
These physical changes, combined with hormonal shifts that affect brain chemistry, create significant challenges for maintaining sexual desire. Fortunately, medical solutions exist to address these hormone-related changes and restore sexual wellness.
What Medical Solutions Can Restore Your Sexual Desire?
Hormone Replacement Therapy Provides Direct Relief
Estrogen therapy remains the most effective treatment for menopause-related sexual desire issues. Transdermal estrogen patches deliver consistent hormone levels and avoid liver metabolism, which makes them safer than oral forms for most women over 50. Studies show that estrogen therapies that produce periovulatory levels of estradiol significantly increase sexual desire in postmenopausal women within 8-12 weeks of treatment.
Testosterone therapy can enhance estrogen’s effects, though the FDA has not approved any androgen therapies specifically for women. Off-label testosterone prescriptions require careful monitoring because supraphysiological doses can cause unwanted side effects like voice changes and increased body hair. Doctors recommend starting with bioidentical hormones at the lowest effective dose and adjusting based on symptom relief and lab results.
Natural Approaches Support Hormonal Balance
Regular exercise increases testosterone production and improves circulation to sexual organs. Strength training shows particularly strong effects on hormone levels. Physical activity is associated with improved psychological well-being in young adults, which can positively impact overall sexual health.
Adequate sleep directly affects hormone production. Women who get less than 6 hours nightly show 15% lower testosterone levels than those who sleep 7-9 hours. Stress management through meditation or yoga reduces cortisol levels that interfere with sex hormone production.
Nutritional Support Enhances Hormone Function
Omega-3 fatty acids from fish oil support hormone synthesis throughout the body. Zinc supplementation can boost testosterone in deficient women, while vitamin D deficiency correlates with reduced sexual desire in multiple studies.
A Mediterranean diet rich in healthy fats, lean proteins, and antioxidants provides the building blocks your body needs for optimal hormone production. Women who follow this eating pattern show more stable hormone levels compared to those who eat processed foods regularly.
Professional Medical Evaluation Identifies Root Causes
Schedule medical evaluation if sexual desire problems persist for more than three months or significantly impact your relationships. Blood tests that measure estradiol, total testosterone, free testosterone, and thyroid hormones identify specific deficiencies that require treatment.
Women who experience sudden libido loss, painful intercourse, or complete absence of sexual thoughts need immediate medical attention to rule out serious underlying conditions. A comprehensive female hormone optimization approach can address the complex interplay of hormones affecting sexual desire. Antidepressants, blood pressure medications, and antihistamines commonly suppress sexual desire and may require dosage adjustments or alternative treatments.
Final Thoughts
Your hormones and female libido work together in complex patterns that change throughout your life. Women who track their menstrual cycles identify when sexual desire naturally peaks and dips, which provides valuable insights into their body’s rhythms. This knowledge helps you predict and manage changes in your sexual interest more effectively.
Sexual health problems don’t resolve themselves without intervention. When hormonal imbalances affect your intimate relationships for more than three months, professional medical evaluation becomes necessary. Blood tests reveal specific hormone deficiencies that targeted treatments can address effectively.
We at Mosaic Medicine Clinic provide comprehensive hormone optimization services that address estrogen, testosterone, and other hormones that affect your sexual wellness. Modern medicine offers proven solutions for hormone-related sexual health issues, from bioidentical hormone replacement to lifestyle modifications that support natural hormone production. Taking action now prevents these problems from worsening and helps you reclaim the intimate wellness you deserve.