Women face distinct mental health challenges that often go unrecognized or unsupported. Depression and anxiety affect women at significantly higher rates than men, yet many struggle in silence without adequate resources or understanding.
At Mosaic Medicine Clinic, we believe that supporting female mental health requires both practical strategies and systemic change. This guide offers concrete steps you can take-whether you’re supporting yourself, a loved one, or creating healthier environments in your workplace and home.
Understanding Why Women Face Higher Mental Health Risks
Depression and Anxiety Strike Women at Twice the Rate
Depression affects women at higher rates than men, with major depressive episodes occurring in 10.3% of adult females compared to 6.2% of adult males. Anxiety follows a similar pattern. This gap translates to millions of women experiencing conditions that fundamentally disrupt their daily lives, relationships, and work. Women make up the majority of those diagnosed with eating disorders, and trauma exposure leaves them about twice as likely as men to develop PTSD. The Office on Women’s Health reports that women experience persistent sadness, fatigue, and feelings of worthlessness at higher rates, often accompanied by physical symptoms like headaches.
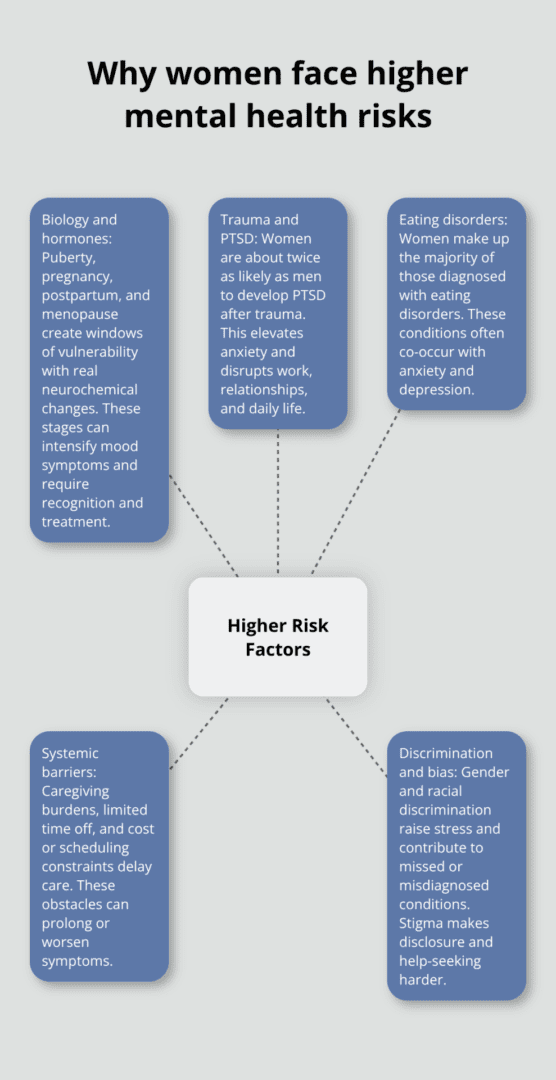
Around 1 in 5 women experience mental disorders globally. This pattern reflects specific vulnerabilities rooted in biology and circumstance-not weakness, but real differences that demand real attention.
Hormonal Shifts Destabilize Mental Health Across Life Stages
Hormonal changes trigger measurable shifts in brain chemistry throughout a woman’s life. Puberty, pregnancy, the postpartum period, and menopause each create windows of vulnerability. Premenstrual dysphoric disorder affects roughly 1 in 20 women with symptoms severe enough to disrupt daily functioning. Postpartum depression impacts more than 10 percent of new mothers, yet many suffer without diagnosis because symptoms get dismissed as baby blues. The NHS notes that menopause can reignite mood symptoms for some women, compounded by midlife stressors and changing social roles. These aren’t minor fluctuations-they represent real neurochemical events that require recognition and treatment.
Systemic Barriers Block Access to Care and Support
Women face pressures that create concrete obstacles to mental health treatment. The Kaiser Family Foundation found that about 1 in 4 women cannot take time off work for mental health care-a barrier that traps women in cycles of untreated illness. Domestic abuse affected 1.6 million women in England and Wales in 2021, and the World Health Organization confirms that abuse directly correlates with depression, anxiety, and self-harm risk. Women shoulder caregiving responsibilities at disproportionate rates, which the Office on Women’s Health links to depression, sleep problems, irritability, and social isolation. Infertility and pregnancy loss carry profound psychological weight, yet specialized support remains limited in many communities. About 1 in 4 women postpone or skip mental health treatment due to cost or scheduling conflicts.
Discrimination Compounds Mental Health Challenges
Gender discrimination and systemic inequities amplify mental health struggles. Racial discrimination intersects with gender to create heightened stress responses and worse mental health outcomes. Healthcare providers sometimes miss or misdiagnose women’s mental health conditions, particularly when symptoms present differently than in men or when gender bias influences clinical judgment. Stigma surrounding mental health remains stronger for women in many contexts, making disclosure harder and help-seeking riskier. These barriers operate at the system level-they reflect structural problems, not personal failings. Addressing them requires both individual action and structural change.
Understanding these challenges sets the stage for practical solutions. The next section explores concrete strategies that actually work to support female mental health and wellbeing.
What Actually Works to Support Female Mental Health
Build Real Social Connections
Social connection forms the foundation of women’s mental health-it’s not optional. The Office on Women’s Health emphasizes that time with loved ones and active social engagement directly improves wellbeing, yet many women isolate when they struggle most. A six-year study published in MDPI Healthcare tracked 12 women through a personal development group program and found that group participation created lasting improvements in self-esteem, emotional expression, and resilience. Participants described the group as a second family that sustained benefits long after the formal program ended.
Women often manage multiple relationships as partners, mothers, and caregivers while neglecting their own peer connections. Identify one consistent social commitment: a weekly coffee with a friend, a monthly book club, or a community group focused on something you genuinely care about. Quality matters more than frequency. One meaningful conversation with someone you trust does more for your mental health than surface-level interactions with many people. If traditional social groups feel overwhelming, online communities focused on specific interests work too, though research from the NIH suggests limiting social media time to avoid negative mood impacts while maintaining genuine connection.
Practice Concrete Stress Management
Stress management requires specificity, not vague self-care advice. The Office on Women’s Health recommends concrete daily practices: 30 minutes of regular exercise most days, consistent sleep schedules, eating nutritious food, limiting caffeine and alcohol, and staying hydrated. These aren’t luxuries-they function as neurochemical interventions.

The Greek study found that women who learned specific stress management techniques like guided imagery and deep breathing applied these tools during actual crises (such as COVID-19), staying calmer and more resourceful when it mattered most.
Set one realistic boundary this week, not five. Many women fail at self-care because they attempt everything simultaneously. Instead, choose one change: move your phone out of the bedroom to improve sleep, or add a 20-minute walk three times weekly. Track what shifts. When you notice real improvement, add one more practice. This incremental approach builds sustainable habits rather than overwhelming yourself with unrealistic expectations.
Access Professional Support When You Need It
Professional help deserves the same directness as other health interventions. If you experience persistent sadness, trouble sleeping, appetite changes, irritability, or thoughts of self-harm, talk with a healthcare provider about treatment options rather than waiting for symptoms to worsen. Treatment works-therapy, medication, or both address the neurochemical and relational roots of depression and anxiety.
Cost and time remain barriers for one in four women, so ask your provider about options: some offer sliding scales, teletherapy reduces travel time, and employee assistance programs through work provide free confidential counseling. If you’re in crisis, contact 988 (Suicide and Crisis Lifeline) by calling, texting, or chatting at 988lifeline.org-it’s confidential and available 24/7. These practical support systems exist specifically to meet women where they are, removing common obstacles to care.
The strategies above work best when they operate within environments that actively support female mental health. Creating those environments-at work, at home, and in your community-requires recognizing the signs that someone struggles and building systems that encourage honest conversation.
Building Environments Where Women’s Mental Health Matters
Notice the Signs Others Miss
Recognizing that someone struggles with mental health requires you to notice what others miss. Women often hide depression and anxiety behind competence at work or caregiving at home, so the signs appear subtle. Watch for persistent fatigue that sleep doesn’t fix, withdrawal from activities they once enjoyed, irritability that feels disproportionate to circumstances, or comments about feeling worthless or hopeless. The Office on Women’s Health notes that women experiencing mental health challenges often report physical symptoms first-chronic headaches, digestive problems, or unexplained pain-because discussing mood feels safer than admitting emotional distress.
When a colleague misses deadlines repeatedly, a friend cancels plans constantly, or a family member stops engaging in conversations, these patterns matter more than any single incident. At work, managers should notice when high performers suddenly produce lower quality work or when reliable team members become withdrawn. At home, partners notice sleep disruption, appetite changes, or emotional flatness. These observations only help when you act on them, not when you notice and stay silent. The most dangerous assumption is that someone will ask for help-they rarely do without invitation.
Start Direct Conversations
Once you notice someone struggling, the conversation itself becomes your intervention. Start with directness rather than hints: say what you’ve observed without judgment, then ask an open question. Instead of hoping they’ll mention their stress, try saying directly, “I’ve noticed you seem withdrawn lately. Is everything okay?” This specificity works because it removes the burden of disclosure-you’ve already named the concern.

Barriers to mental health care include not just cost and time but also shame and uncertainty about whether help is appropriate. When you normalize mental health conversations in your environment, you remove that barrier. At work, leaders should discuss mental health in team meetings, share their own experiences with stress or therapy, and explicitly state that seeking support is valued rather than penalized.
Make Mental Health Part of Regular Check-Ins
Managers should ask about wellbeing during one-on-one meetings and mean it-not as a perfunctory question but as genuine inquiry. At home, regular check-ins work better than waiting for crises. Ask specifically: “How are you managing your stress? Are you sleeping? Do you need help with anything?” These questions signal that you notice and care.
Women in particular respond to this direct approach because it contradicts the cultural message that struggling alone is stronger than asking for support. The goal isn’t to become a therapist but to be the person who notices, asks, and connects someone to actual help.
Connect People to Professional Resources
When someone discloses mental health struggles, know where to direct them. The Suicide and Crisis Lifeline at 988lifeline.org provides resources for these conversations, including guidance on what to say when someone discloses thoughts of self-harm. At work, your employee assistance program offers confidential support and often includes consultation for managers navigating these conversations-use that resource rather than managing alone.
If you’re unsure how to respond or what to say next, these professional resources exist specifically to support you in supporting others. They remove the pressure to have all the answers while ensuring the person receives appropriate care.
Final Thoughts
Supporting female mental health requires action, not passive hope. Start with one change this week-a 20-minute walk, a conversation with someone you trust, or an appointment with a healthcare provider. If you support others, notice what you’ve overlooked and ask directly about their wellbeing. If you shape workplace or home environments, normalize mental health conversations and remove the barriers that keep women isolated.
Female mental health improves when women stop managing alone and when the people around them actively support rather than ignore their struggles. This means noticing when someone withdraws, recognizing that physical symptoms sometimes signal emotional distress, and understanding that hormonal changes create real neurochemical shifts. It means connecting people to resources, having difficult conversations, and building systems that prioritize wellbeing.
We at Mosaic Medicine Clinic understand that quality healthcare means addressing the whole person, including mental health. If you want a healthcare partner who takes time to understand your needs and connects you with appropriate support, visit Mosaic Medicine Clinic to learn how our Direct Primary Care approach prioritizes your wellbeing. For immediate crisis support, contact 988 (Suicide and Crisis Lifeline) by calling, texting, or visiting 988lifeline.org.