Women’s reproductive health depends on getting the right nutrients at the right time. Whether you’re planning to conceive, managing a cycle condition, or supporting overall wellness, supplements for female reproductive health can make a real difference when chosen wisely.
At Mosaic Medicine Clinic, we’ve seen how the right supplement strategy transforms outcomes for our patients. This guide walks you through evidence-based options, common pitfalls, and how to work with your healthcare provider to build a plan that actually works for your body.
Essential Nutrients for Female Reproductive Health
Iron: The Foundation for Cycle Health and Egg Quality
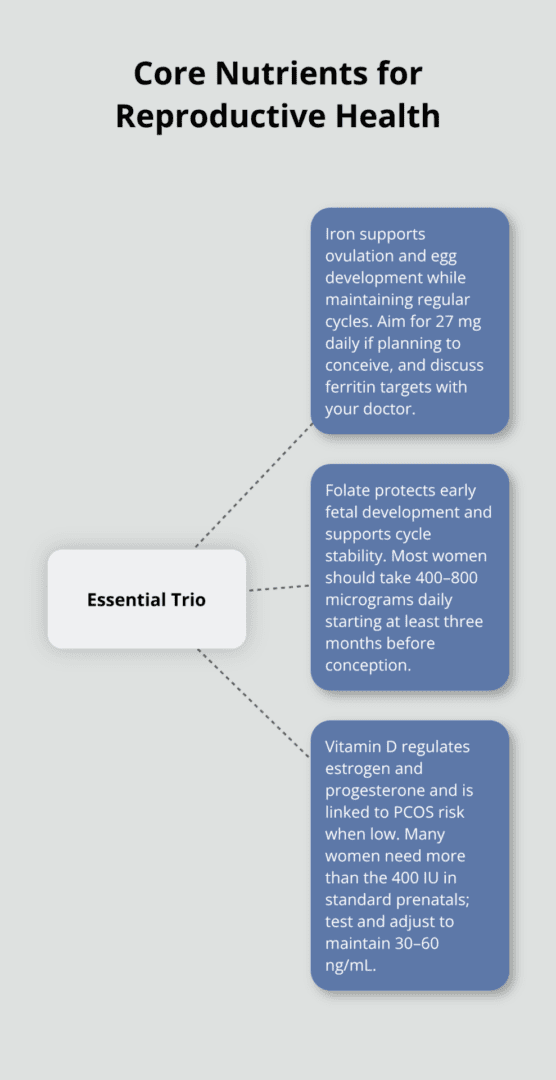
Iron deficiency silently undermines fertility in ways most women don’t recognize until they struggle to conceive. Menstrual blood loss depletes iron stores month after month, and low iron directly impairs egg quality and ovulation. Your eggs need adequate iron to develop properly and your body needs it to maintain a regular cycle. If you plan to conceive, try for 27 mg daily through diet or supplementation, especially if you experience heavy periods. Red meat, lentils, and fortified cereals provide dietary iron, but many women benefit from a supplement to reach therapeutic levels. Testing your iron and ferritin levels with your doctor gives you a baseline; many reproductive health specialists recommend ferritin above 30 ng/mL for optimal fertility outcomes.
Folate: Protection That Starts Before Pregnancy
Folate, the natural form of folic acid, is non-negotiable for anyone thinking about pregnancy. Folic acid supplementation reduces the risk of neural tube defects by up to 60 percent, and this protection begins in the first weeks of pregnancy-often before you know you’re pregnant. This is why the recommendation exists for all women of reproductive age to take 400 to 800 micrograms daily, not just those actively trying.

Beyond preventing birth defects, folic acid stabilizes menstrual cycles and research suggests it may support reproductive health. Start supplementing at least three months before attempting conception; your body needs time to build adequate folate stores.
Vitamin D: The Hormone Regulator That Changes IVF Outcomes
Vitamin D represents the third pillar, and its impact on reproductive outcomes is substantial. Vitamin D supports ovarian follicle function, helps regulate estrogen and progesterone, and deficiency is linked to PCOS development. The Endocrine Society recommends maintaining levels between 30 and 60 ng/mL, though many standard prenatal vitamins contain only 400 IU-insufficient for most women. Many reproductive specialists recommend up to 2,000 IU daily depending on baseline levels, and testing your vitamin D status should happen before you start trying to conceive.
These three nutrients work together to support regular cycles and healthy eggs. Once you establish this foundation, the next layer of your supplement strategy addresses specific reproductive challenges that many women face.
Which Supplements Actually Improve Egg Quality and Cycle Health
CoQ10: Powering Your Eggs’ Energy Production
CoQ10 stands out as the supplement with the strongest evidence for improving egg quality, particularly for women over 35 or those with diminished ovarian reserve. Your eggs are energy-intensive cells, and CoQ10 supports the mitochondria that power egg development. Studies show that women taking 400 to 600 mg daily before IVF retrieve more eggs and produce higher-quality embryos. One analysis found that adequate CoQ10 levels increased pregnancy rates during fertility treatment and reduced the medication doses needed for ovarian stimulation. Start supplementing at least three months before attempting conception, since eggs develop over a 90-day cycle. The ubiquinol form of CoQ10 absorbs more effectively than standard ubiquinone, so check your supplement label carefully. If you have low ovarian reserve or are over 35, this supplement deserves a spot in your regimen.
Inositol: Restoring Insulin Sensitivity for PCOS
Inositol addresses a different reproductive challenge entirely, making it essential for women with PCOS. Myo-inositol and D-chiro-inositol work together to restore insulin sensitivity, which directly improves ovulation rates and egg quality. Research shows that inositol can increase ovulation and pregnancy rates comparable to or better than metformin in PCOS, without the digestive side effects many women experience. The typical dose ranges from 2 to 4 grams daily, and combining inositol with folic acid may further enhance fertilization and pregnancy rates during fertility treatment. Women with PCOS who take inositol often see menstrual cycle improvements within two to three months.
Omega-3 Fatty Acids: Reducing Inflammation and Supporting Hormonal Balance
Omega-3 fatty acids complete this trio by supporting cycle regularity and reducing inflammation in the reproductive system. Try 1,000 mg of DHA daily, which supports hormonal balance and may improve ovarian function. Algae-based omega-3 sources work well for vegetarians, and pairing omega-3s with a balanced omega-6 intake matters more than most women realize.
Finding Your Personalized Supplement Strategy
These three supplements address distinct mechanisms: egg energy production, insulin resistance, and systemic inflammation. Your healthcare provider can help you determine which ones match your specific reproductive health needs and baseline health status. The next section covers the mistakes that derail even well-intentioned supplement strategies, so you can avoid the pitfalls that prevent real results.
Common Mistakes That Sabotage Your Supplement Strategy
Starting Supplements Without Medical Guidance
The single biggest mistake women make is adding supplements without their doctor’s input, and it derails results before they even begin. Many women assume that because supplements are natural, they’re universally safe and effective for everyone. This assumption costs time and money. Your reproductive health exists within a complex system affected by your age, cycle length, hormone levels, underlying conditions like PCOS or thyroid disease, and medications you already take. A supplement that helps one woman may be ineffective or even harmful for another.
CoQ10 works brilliantly for women over 35 with diminished ovarian reserve, but it won’t improve outcomes for women with normal egg reserves. Inositol transforms menstrual regularity in PCOS, yet offers no benefit for women without insulin resistance.

Before you add any supplement to your regimen, get baseline testing done. Your doctor should measure your iron, ferritin, vitamin D, and thyroid function. These numbers tell you exactly what your body actually needs rather than what marketing promises. Without this foundation, you’re essentially guessing, and guessing wastes months you could spend on interventions that actually work for your specific situation.
Overlooking Medication and Supplement Interactions
Medication interactions and overlooked contraindications create a second major problem that most women never anticipate. High-dose vitamin D can interact with certain blood pressure medications and increase calcium absorption in ways that matter if you have kidney disease or heart conditions. CoQ10 may thin blood slightly, which matters if you take anticoagulants. Inositol can lower blood sugar, requiring dose adjustments if you take diabetes medications. Iron supplements reduce absorption of certain antibiotics and thyroid medications, meaning timing matters significantly.
Many women take supplements without telling their doctor because they don’t think it’s relevant, then wonder why their medications stop working as expected. Your pharmacist can run an interaction check, but only if they know about every supplement you’re taking. Write down everything before your appointment, including doses and frequency. This simple step prevents costly complications and wasted effort.
Expecting Supplements to Replace Lifestyle Foundations
The final mistake involves expecting supplements to compensate for poor lifestyle choices. Supplements amplify what you’re already doing; they don’t replace it. A woman taking CoQ10 while sleeping five hours nightly won’t see the egg quality improvements that studies document. Iron supplementation won’t restore cycle regularity if you’re under chronic stress without management strategies. Omega-3s won’t reduce inflammation if your diet remains high in processed foods.
Supplements work best when combined with adequate sleep, consistent exercise, stress management, and a nutrient-dense diet. This combination drives real reproductive health outcomes, not supplements alone. Your healthcare provider can help you assess whether your current lifestyle supports your supplement strategy and identify which areas need attention first.
Final Thoughts
The evidence shows that supplements for female reproductive health work best when you choose them based on your individual needs, not marketing claims or what worked for your friend. Iron, folate, and vitamin D form the foundation that every woman should address before adding anything else. CoQ10 makes sense if you’re over 35 or have diminished ovarian reserve, while inositol transforms outcomes for women with PCOS. Omega-3s support cycle regularity and hormonal balance across the board.
Start by getting tested to know your iron, ferritin, vitamin D, and thyroid levels before you spend money on supplements that might not address your actual deficiencies. Talk to your doctor about any medications you take and any supplements you’re considering, because interactions happen quietly and derail your progress. Build your supplement strategy on a foundation of adequate sleep, consistent movement, stress management, and real food-supplements amplify what you’re already doing, they don’t replace the basics.
We at Mosaic Medicine Clinic understand that reproductive health decisions feel personal and urgent. Our approach focuses on unrushed appointments and direct access to physicians who can review your labs, assess your specific situation, and build a plan tailored to you. If you’re ready to work with a healthcare provider who takes supplements seriously and integrates them into comprehensive reproductive health care, connect with us at Mosaic Medicine Clinic.