Men experiencing unexplained fatigue, mood swings, or mental fog often dismiss these changes as normal aging. Yet these could be signs of andropause symptoms that deserve medical attention.
At Mosaic Medicine Clinic, we see many men surprised to learn their declining energy and cognitive changes stem from dropping testosterone levels. Understanding these signs can lead to proper diagnosis and treatment.
What Makes Andropause Different from Female Menopause
The Gradual Testosterone Drop
Andropause represents a slow, steady decline in testosterone production that begins around age 30, with levels dropping approximately 1.6% annually. This gradual process affects an estimated 5 million men in the United States, with testosterone levels potentially falling by 50% at age 70 compared to peak levels. The Mayo Clinic confirms that 10% to 15% of men over 60 experience clinically low testosterone, with percentages rising as men age further.

Why Male Hormonal Changes Are Harder to Detect
The fundamental difference between andropause and female menopause lies in timing and intensity. Women experience a rapid, complete shutdown of hormone production over months, while men face decades of gradual decline that starts in their thirties. This slow progression means symptoms often get dismissed as normal aging, which makes diagnosis challenging. Men’s reproductive systems never completely shut down like women’s do during menopause, which explains why symptoms vary dramatically between individuals.
When Testosterone Levels Become Problematic
Normal testosterone ranges between 275 to 900 nanograms per deciliter (ng/dL), with levels below 275 ng/dL considered deficient. Testing should occur between 7 a.m. and 10 a.m. after fasting for accurate results. Weight gain, chronic illness, stress, and certain medications accelerate testosterone decline beyond the typical 1-2% annual drop. Men with obesity or type 2 diabetes face higher risks of developing late-onset hypogonadism, which makes lifestyle factors important in determining symptom severity.
Physical and Mental Signs of Andropause That Often Get Overlooked
Many men don’t recognize the subtle symptoms that develop over years of testosterone decline. These overlooked signs often masquerade as stress or normal aging, which leads to delayed diagnosis and treatment.
What Surprising Symptoms Signal Andropause
Energy Crashes That Don’t Match Your Sleep
Men with dropping testosterone levels experience persistent fatigue that sleep doesn’t fix. This isn’t the tired feeling after a long workday – it’s bone-deep exhaustion that makes simple tasks feel overwhelming. Late-onset testosterone deficiency in early middle-aged men (40-49 years) is increasingly recognized and is often associated with obesity, yet most attribute it to work stress or poor sleep habits.
Sleep disturbances compound the problem. Men with low testosterone frequently wake up multiple times during the night, experience restless sleep, and feel unrefreshed despite spending 7-8 hours in bed. Sleep apnea affects testosterone production and creates a cycle where poor sleep lowers testosterone, which then disrupts sleep quality further.
Brain Fog and Emotional Changes That Creep Up Slowly
Testosterone decline creates cognitive changes that men rarely connect to hormones. Concentration problems, memory lapses, and difficulty with decisions develop gradually over months or years. Men report that their mental sharpness has dulled, with tasks that once felt automatic now requiring extra effort and focus.
Mood swings, irritability, and loss of motivation often accompany these cognitive changes. Depression affects many men with low testosterone, though doctors overlook the connection because symptoms develop slowly. Men may lose interest in activities they previously enjoyed, feel less confident, or experience unexplained anxiety. These psychological symptoms frequently prompt men to seek mental health treatment when hormone evaluation might provide more targeted solutions.
Physical Changes Beyond Sexual Function
Weight gain around the midsection occurs because testosterone helps regulate fat distribution and muscle mass. Men notice their body composition changes – they lose muscle tone while gaining belly fat, even without major diet or exercise changes. This abdominal weight gain contains aromatase enzymes that convert remaining testosterone into estrogen and accelerate the hormone imbalance.
Decreased bone density, thinning skin, and reduced body hair growth represent less obvious physical changes. Some men develop gynecomastia (breast tissue enlargement) due to shifting hormone ratios. Reduced morning erections and changes in orgasm intensity often serve as early indicators, though men frequently dismiss these as normal aging rather than recognize them as hormone-related symptoms.
When These Symptoms Warrant Medical Attention
These symptoms often develop so gradually that men adapt to them without realizing their quality of life has declined. The key lies in recognizing when multiple symptoms appear together or when they significantly impact daily activities, relationships, or work performance. Proper testing can determine whether these changes stem from testosterone deficiency or other underlying health conditions.
How Do You Get Tested for Low Testosterone?
Schedule Your Test at the Right Time
Testosterone tests require precise timing for accurate results. Schedule your blood draw between 7 a.m. and 10 a.m. after you fast overnight, as testosterone levels are sleep-dependent and require at least 3 hours of sleep with normal architecture to increase properly. Avoid tests when you’re sick, stressed, or take medications that could affect hormone levels. Most doctors require two separate morning tests that show low levels before they diagnose testosterone deficiency, since levels can fluctuate due to sleep, illness, or stress.

Find the Right Healthcare Provider
Primary care physicians can order initial testosterone tests, but many lack specialized training in hormone therapy. Endocrinologists and urologists have deeper expertise in testosterone deficiency diagnosis and treatment options. Men’s health specialists understand the nuanced symptoms and can connect physical changes to hormone levels more effectively than general practitioners. Many men receive incomplete evaluations elsewhere and need comprehensive hormone assessment to identify the root causes of their symptoms.
Additional Tests That Reveal the Complete Picture
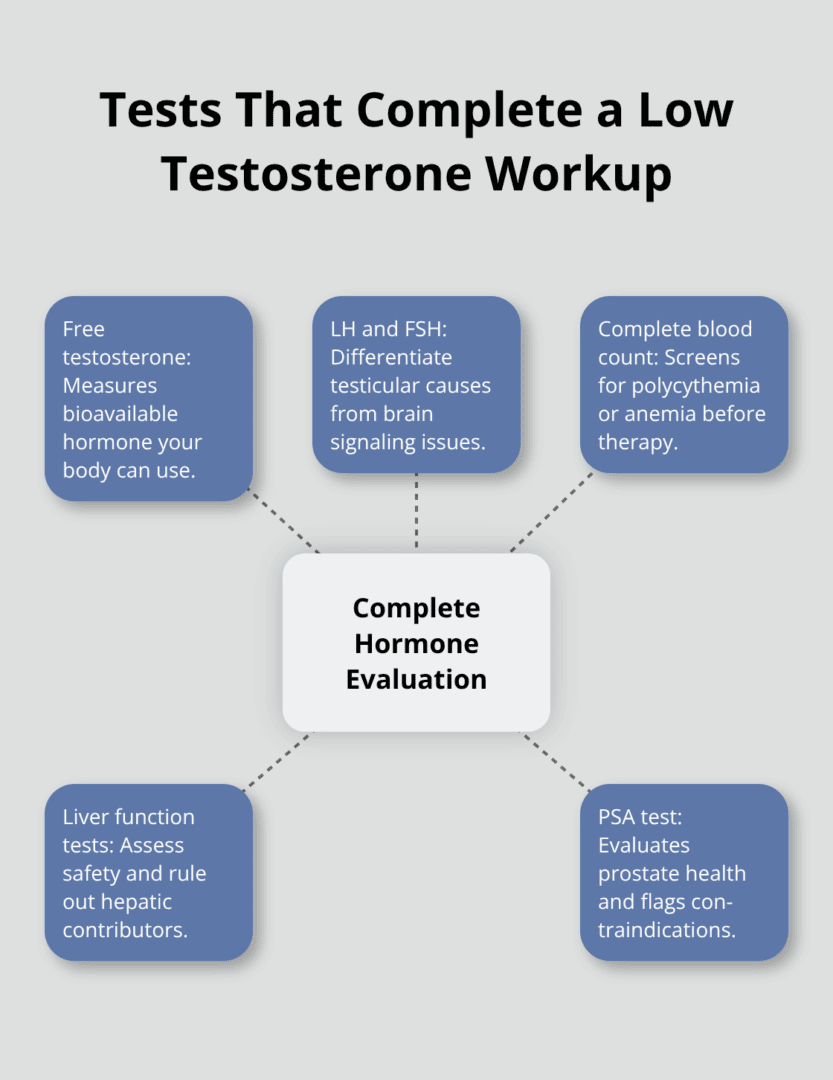
Beyond total testosterone, doctors should test free testosterone, which measures the hormone available for your body to use. Luteinizing hormone (LH) and follicle-stimulating hormone (FSH) tests determine whether low testosterone stems from testicular problems or brain signaling issues. Complete blood count, liver function, and prostate-specific antigen (PSA) tests rule out underlying conditions that could cause symptoms or contraindicate treatment.
What Your Test Results Mean
Normal testosterone ranges between 264 to 916 nanograms per deciliter (ng/dL) for non-obese men aged 19-39, with levels below this range considered deficient. However, symptoms can occur even when levels fall within the lower normal range. Your doctor will evaluate your symptoms alongside your test results rather than rely solely on numbers. Age-related decline means that a 50-year-old man with 350 ng/dL might experience symptoms, while the same level might feel normal for a 70-year-old.
Prepare for Your Appointment
Bring a detailed list of your symptoms, including when they started and how they affect your daily life. Note any medications, supplements, or health conditions that might influence testosterone levels. Track your sleep patterns, energy levels, and mood changes for several weeks before your appointment. This information helps your doctor understand the full picture and determine whether testosterone deficiency explains your symptoms or if other conditions require investigation.
Final Thoughts
Andropause symptoms extend far beyond sexual health concerns and often appear as normal aging. Persistent fatigue that sleep doesn’t resolve, brain fog, mood changes, unexplained weight gain around the midsection, and muscle mass decline deserve medical attention rather than acceptance as inevitable changes. The gradual nature of testosterone decline makes these symptoms easy to dismiss, yet they significantly impact quality of life, relationships, and work performance.
Men who experience multiple symptoms together should seek proper evaluation rather than struggle through changes that may have effective treatments. Testing requires morning blood draws and evaluation by healthcare providers experienced in hormone health. Treatment options range from lifestyle modifications like weight loss and exercise to testosterone replacement therapy (depending on individual circumstances and underlying causes).
We at Mosaic Medicine Clinic understand that men’s health concerns require comprehensive evaluation and personalized treatment approaches. Our Direct Primary Care model allows for thorough assessments and ongoing support as you address hormone-related health changes. Don’t let these symptoms define your future when effective solutions may be available.











