Your doctor has seven minutes to address your concerns before rushing to the next patient. You wait weeks for appointments, then receive bills you never expected.
At Mosaic Medicine Clinic, we see how traditional healthcare systems leave patients frustrated and underserved. Personalized healthcare offers a better path forward. The one-size-fits-all approach simply doesn’t work when every person has unique health needs and goals.
Why Traditional Healthcare Wastes Your Time and Money
Traditional healthcare systems trap patients in cycles of inefficiency and frustration that damage both health outcomes and financial stability. The average American waits 24 days for routine appointments with primary care physicians, according to Merritt Hawkins medical survey data. Once you arrive, physicians spend just 13 to 16 minutes with each patient during office visits, as the American Medical Association reports.
The Seven-Minute Reality
Primary care doctors face impossible pressures that force them to rush through appointments. Many physicians see 25 to 30 patients daily to meet revenue targets that healthcare systems set. This assembly-line approach prevents doctors from addressing multiple health concerns, understanding your complete medical history, or developing comprehensive treatment plans. Patients leave appointments with unanswered questions and unresolved symptoms because thorough care takes time that doesn’t exist.

After-Hours Healthcare Desert
When health concerns arise outside business hours, patients face limited options that often lead to expensive emergency room visits. Emergency departments experience significant wait times, with costs that average $1,389 per visit (according to Health Affairs research). Most traditional practices offer no direct communication with physicians, which forces patients to navigate phone trees, leave messages with staff, or wait until the next available appointment days or weeks later.
Financial Surprise Attacks
Healthcare bills create financial chaos for patients who cannot predict costs before they receive care. High deductibles and copayments are causing nearly two of five working-age adults to delay visiting the doctor and filling prescriptions. Insurance networks change without notice, labs order tests without price transparency, and specialists bill separately from facilities. These practices create multiple unexpected charges for single episodes of care.
These systemic problems highlight why patients need healthcare models that prioritize their individual needs and circumstances.
Why Your Health Story Matters More Than Statistics
Medical research shows that social determinants significantly impact chronic disease outcomes, according to the World Health Organization. Your genetics, lifestyle, stress levels, work environment, and personal health goals create a unique profile that standard treatment protocols cannot address. The American Diabetes Association now emphasizes individual treatment approaches because identical medications produce vastly different results across patients with the same diagnosis.
Your Body Responds Differently
Warfarin dosing demonstrates how genetic variations affect treatment outcomes. The FDA reports that VKORC1 and CYP2C9 gene variations require dose adjustments that can differ by 300 percent between patients. Cancer immunotherapy success rates vary dramatically based on tumor mutations specific to each patient, with some treatments showing 90 percent response rates in targeted populations while failing completely in others.
Your treatment plan must account for these individual variations rather than follow generic protocols that ignore your biological uniqueness. Standard protocols assume average responses that rarely match real patient experiences.
Relationships Drive Results
Patients who spend adequate time with their physicians show 40 percent better medication adherence rates compared to those who receive rushed care, according to research published in the Journal of General Internal Medicine. Strong patient-doctor relationships reduce emergency room visits by 25 percent and improve preventive care completion by 35 percent.
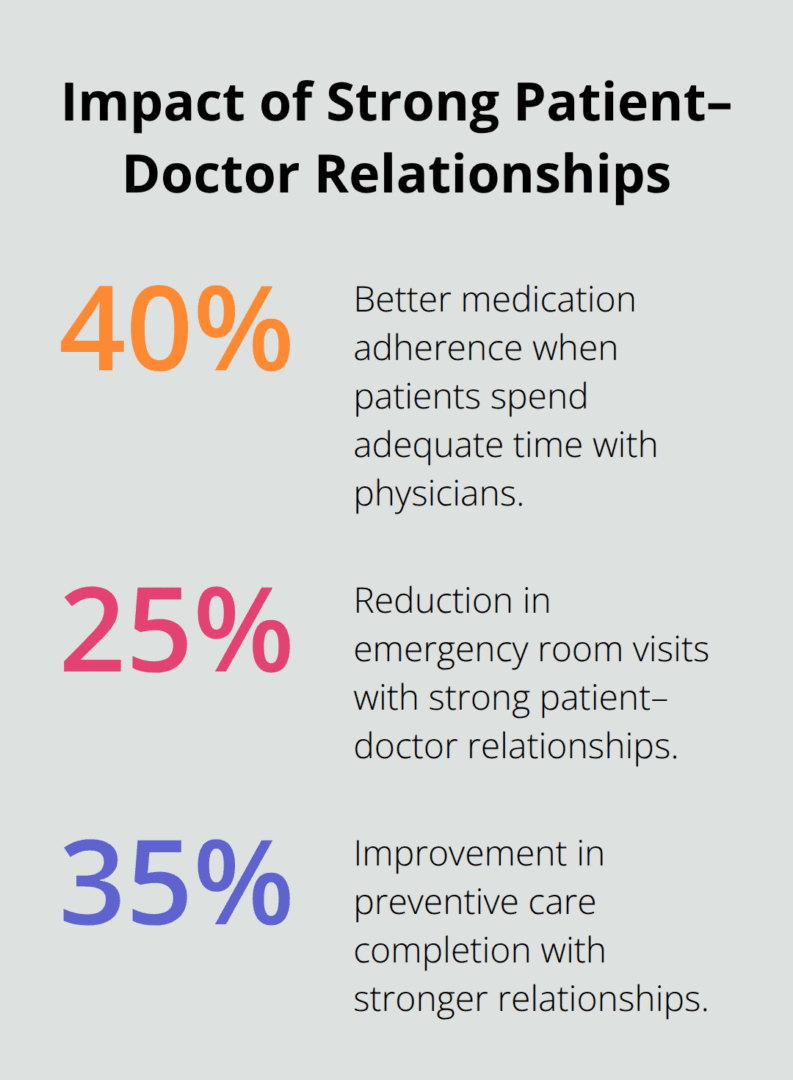
Physicians need meaningful time to understand your health priorities, family history, and lifestyle factors that influence treatment decisions. This comprehensive approach identifies health risks before they become expensive medical emergencies while creating treatment plans that fit your daily routine and personal preferences.
Personal Health Goals Shape Success
Traditional healthcare focuses on disease-specific outcomes that investigators define rather than goals that matter most to patients. Quality of life, personal mobility, and individual health priorities often receive minimal attention in standard treatment protocols. Research from JAMA Internal Medicine advocates for health priorities-tailored care that aligns with what patients actually value.
Your definition of health success may differ significantly from statistical averages that guide standard treatments. Some patients prioritize pain management over longevity, while others focus on maintaining independence rather than following aggressive treatment protocols. These personal preferences should drive medical decisions, not population-wide statistics.
Direct primary care models address these individual needs through extended appointment times and personalized attention that traditional healthcare systems cannot provide.
How Direct Primary Care Fixes Healthcare’s Biggest Problems
Direct primary care transforms healthcare by removing insurance companies from the patient-doctor relationship and creating a membership model that works like a gym or Netflix subscription. DPC practices charge monthly fees that range from $50 to $150 per person, depending on age and services included. This membership provides unlimited office visits, same-day appointments, extended consultation times, and direct communication with physicians through phone calls and secure messages. Primary care has been shown to significantly decrease the overall cost of a population’s health care while improving the quality of each person’s well-being.
Extended Appointments Transform Patient Care
DPC physicians schedule 30 to 60-minute appointments instead of the standard visits that plague traditional practices. Research from the National Ambulatory Medical Care Survey indicates that among general and family physicians, the average visit duration is 18.7 minutes. This extended time allows doctors to address multiple health concerns, review complete medical histories, and develop comprehensive prevention strategies. Physicians in DPC practices typically manage 400 to 600 patients compared to the 2,000 to 3,000 patients that traditional primary care doctors handle. DPC physicians provide significantly more time with patients, which leads to improved chronic disease management and reduced specialist referrals.
Same-Day Access Eliminates Wait Times
DPC practices offer same-day appointments for urgent concerns and maintain open communication channels between visits. Patients reach their physicians directly through secure text messages, phone calls, and email without navigating phone trees or waiting for callbacks. This immediate access prevents minor health issues from becoming major problems that require expensive emergency room visits. Traditional practices force patients to wait weeks for routine appointments, while DPC members schedule visits within 24 hours or less.
Transparent Pricing Eliminates Financial Surprises
DPC practices offer wholesale laboratory tests at 70 to 90 percent below standard retail prices, according to the Direct Primary Care Coalition. Medical facilities provide direct contracts for tests and procedures at 50 to 80 percent below insurance rates. Generic medications often cost $5 to $15 per month instead of the $50 to $200 copayments that insurance plans require.
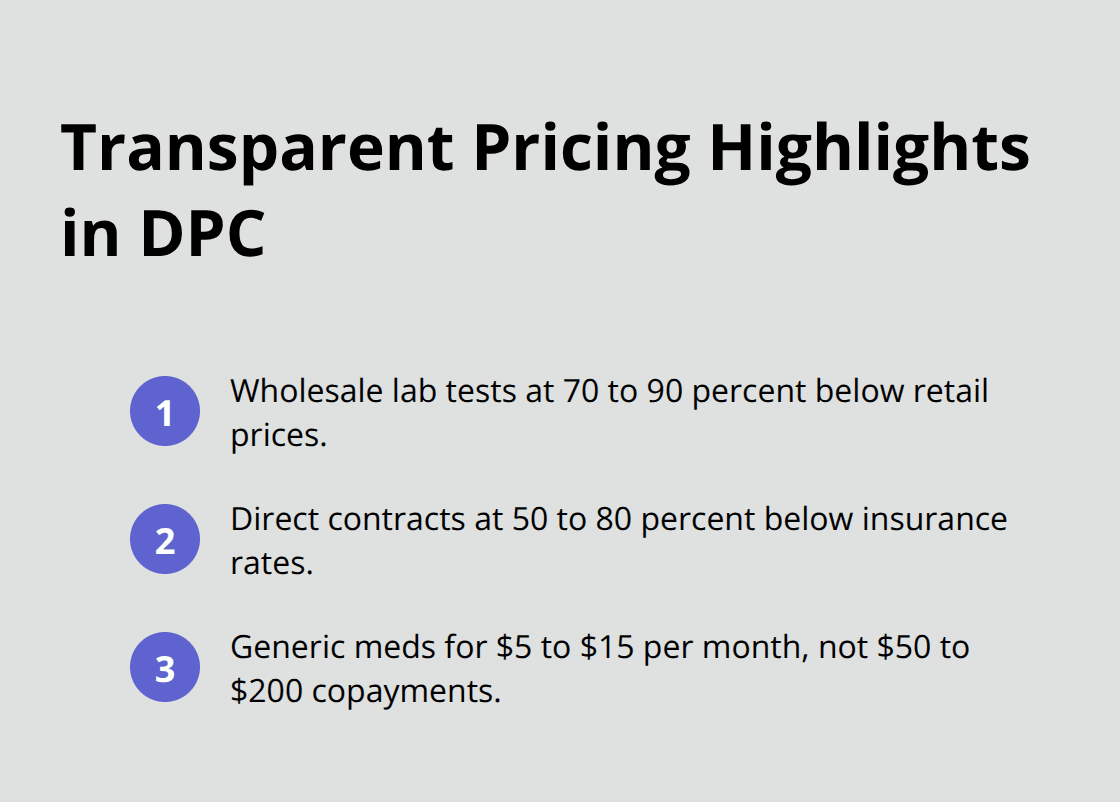

Patients know exact costs before they receive services, which eliminates surprise bills and allows them to budget healthcare expenses accurately. This transparency helps small business healthcare families save thousands of dollars annually while they receive higher-quality care.
Final Thoughts
Traditional healthcare systems fail patients through rushed appointments, limited access, and unpredictable costs that prioritize profits over patient outcomes. The evidence shows that personalized healthcare delivers superior results when doctors address individual health needs, genetic variations, and personal goals that standard protocols ignore. Patients who receive individualized care experience better medication adherence rates and fewer emergency room visits.
Direct primary care practices like Mosaic Medicine Clinic demonstrate how membership-based models transform patient experiences through extended appointments, same-day access, and transparent costs. This approach eliminates insurance complications while doctors provide comprehensive primary care, preventative medicine, and specialized programs that traditional practices cannot offer. Patients know exactly what they pay each month without surprise bills or hidden fees.
Your health deserves more than assembly-line medicine that treats symptoms rather than addresses your complete health picture. Personalized healthcare models create stronger patient-doctor relationships that improve health outcomes and address priorities that matter most to you (quality of life, mobility, and personal wellness goals). The choice between frustrating traditional healthcare or personalized care models that actually work remains yours to make.