Direct patient care experience separates good healthcare providers from great ones. It’s where clinical knowledge meets real human connection, and where you learn what patients actually need beyond what textbooks teach.
At Mosaic Medicine Clinic, we’ve seen firsthand how providers who invest in meaningful patient interactions build stronger practices and deliver better outcomes. Whether you’re early in your career or looking to deepen your clinical foundation, there are proven pathways to gain this experience.
Why Direct Patient Care Experience Shapes Your Career
Clinical Knowledge Meets Real Human Connection
Direct patient care experience fundamentally changes how you understand medicine. When you spend sustained time with patients-taking vitals, assisting with treatments, counseling them through health decisions-you develop clinical judgment that no classroom can teach. Healthcare providers with extensive direct patient contact demonstrate higher diagnostic accuracy and better patient compliance with treatment plans. You learn to recognize subtle changes in patient status, understand how chronic conditions actually affect daily life, and spot the moments when a patient needs more than just medical advice.
This isn’t theoretical knowledge. A patient with diabetes doesn’t just need insulin instructions; they need to understand how medication costs affect their ability to fill prescriptions, how food insecurity impacts their nutrition, and how transportation barriers prevent them from attending follow-up appointments. You only learn these realities through consistent, meaningful interaction with real patients across different settings and socioeconomic circumstances.
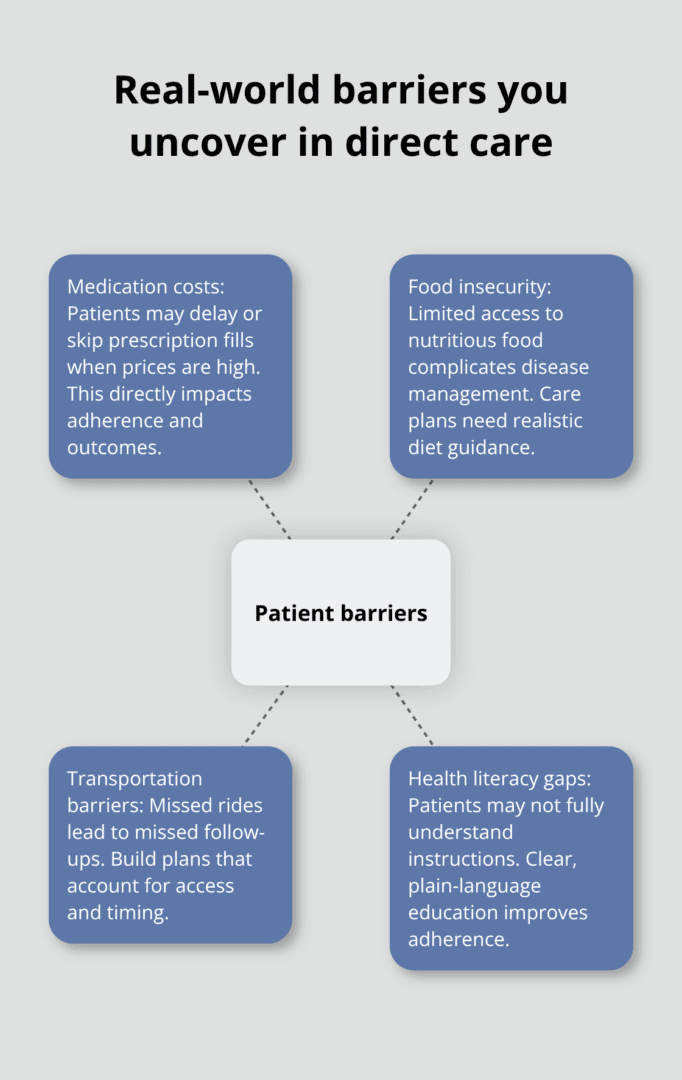
Building Relationships That Improve Outcomes
The relationship between you and your patient becomes the foundation of effective care. When patients see the same provider over time, they share more information, follow recommendations more faithfully, and experience better health outcomes. Extended time with each patient reveals what matters most to them. You learn that your 65-year-old patient’s real concern isn’t just blood pressure control but maintaining independence to care for grandchildren. You find that your young professional’s anxiety about chest pain stems from work stress, not cardiac disease. These insights only emerge when you’re not rushing through a 10-minute appointment slot.
Direct Primary Care practices prioritize unrushed appointments and direct physician access that allows providers to build genuine relationships with their patients. This model works because it removes the time constraints that prevent meaningful connection.
Accelerating Clinical Skill Development
Consistent direct patient care accelerates your clinical skill development faster than any simulation or textbook study. Each interaction teaches you something about disease presentation, patient psychology, and treatment response that textbooks describe in abstract terms. You develop intuition about which patients need aggressive intervention and which need watchful waiting, which complaints signal serious illness and which reflect normal aging. This clinical judgment becomes your most valuable asset as a healthcare provider, and it’s built entirely through accumulated hours of direct patient care.
The skills you gain-from recognizing patterns in vital signs to understanding medication adherence challenges-prepare you to handle the complexity and unpredictability of real clinical work. These competencies form the foundation for the specific pathways and roles that can accelerate your direct patient care experience.
Where to Find Direct Patient Care Opportunities
Direct Primary Care Practices Offer Unrushed Patient Interaction
Direct Primary Care practices stand out as the most intentional setting for building meaningful patient relationships. These membership-based models eliminate the time pressure that plagues traditional fee-for-service medicine. Providers in DPC settings spend 30 to 45 minutes per patient visit instead of the standard 15-minute appointment slots found in conventional practices. The financial structure of DPC removes the incentive to see more patients faster, which fundamentally changes the quality of care you’ll witness and practice.
In a DPC environment, you’ll observe how providers manage chronic disease prevention, handle complex medication interactions, and address the social determinants that textbooks mention but traditional clinics ignore. You’ll see patients return regularly, allowing you to track outcomes over months and years rather than isolated visits. This continuity teaches clinical judgment that acute-care settings cannot provide.

Community Health Centers Expose You to Complex Social Barriers
Volunteer positions at community health centers expose you to underserved populations with complex social and economic barriers to care. You’ll encounter patients managing multiple chronic conditions with limited resources, which teaches practical problem-solving that private practice settings rarely demonstrate. These environments reveal how medication costs affect adherence, how food insecurity impacts nutrition management, and how transportation barriers prevent follow-up care.
The patients you work with in community health settings often navigate healthcare systems with far fewer advantages than insured populations. This exposure shapes your understanding of health equity and teaches you to think creatively about treatment plans that actually work within patients’ real circumstances.
Urgent Care and Specialty Clinics Teach Acute Decision-Making
Urgent care and specialty clinics provide exposure to acute presentations and focused clinical decision-making, though these environments typically involve shorter patient interactions. You’ll learn to recognize patterns in acute illness, make rapid assessments, and implement time-sensitive interventions. These settings teach efficiency and decisiveness that complement the relationship-building skills you develop in primary care environments.
Entry-Level Clinical Roles Deliver Hands-On Patient Contact
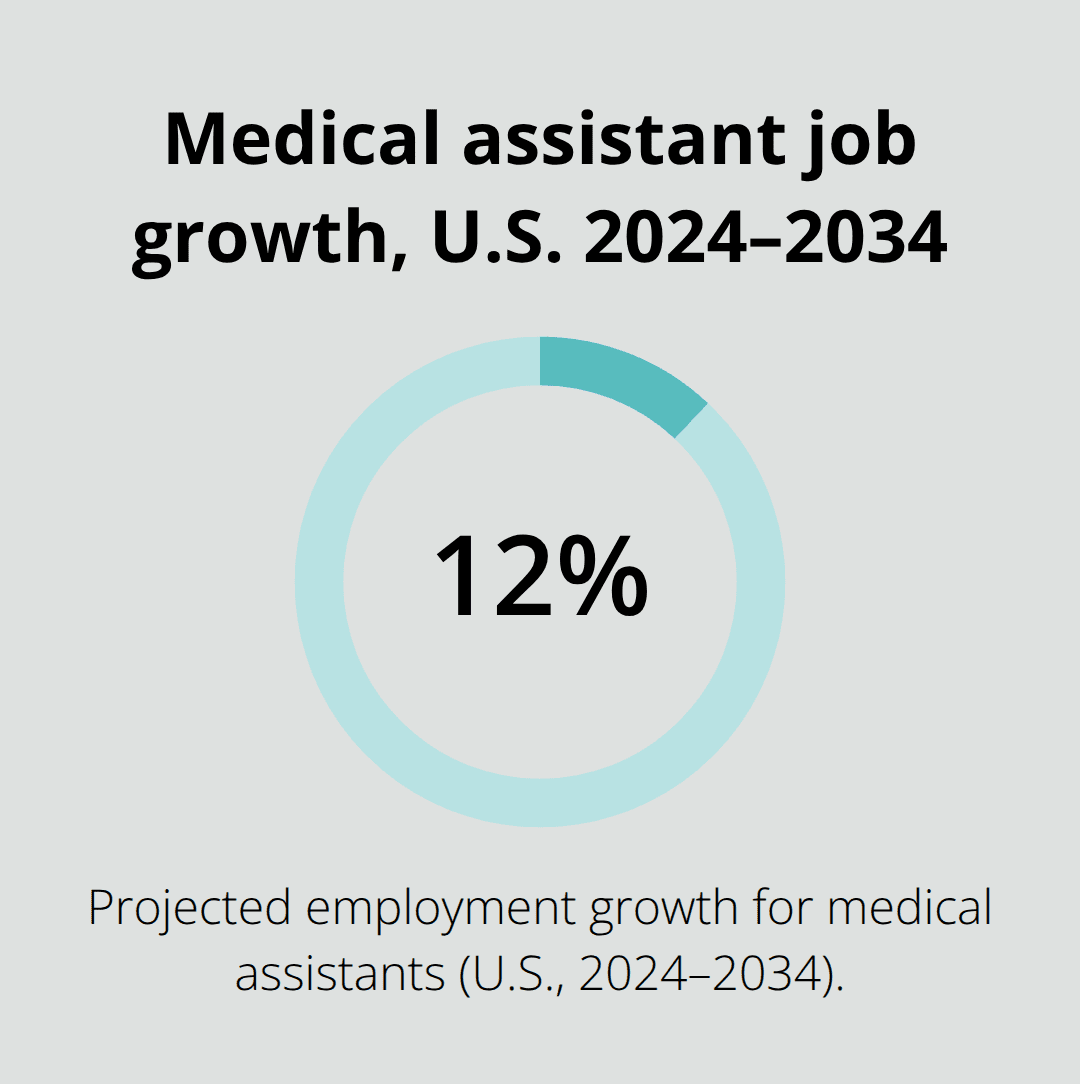
If you’re serious about direct patient care experience, seek positions where you actually deliver care-not shadow or document-through roles like medical assistant, patient care technician, or phlebotomist. Employment of medical assistants is projected to grow 12 percent from 2024 to 2034, much faster than the average for all occupations, making these entry points both accessible and increasingly available. Community colleges and vocational programs offer 4 to 16-week CNA training programs that position you for immediate hands-on work in hospitals and clinics.
These roles place you directly in patient care workflows. You touch patients, assist with treatments, and observe how clinical decisions translate into real outcomes. This hands-on experience accelerates your clinical development far faster than observation-only positions.
The Critical Difference: Active Care Versus Passive Observation
The key distinction between valuable experience and wasted time is whether you’re actively involved in patient care, making decisions about their care, and reflecting on outcomes. Shadowing teaches you what medicine looks like; direct patient care teaches you what medicine feels like and how to practice it. The next section explores how to extract maximum learning from whatever direct patient care setting you enter.
How to Turn Patient Care Into Patient Learning
Document every significant patient encounter
Direct patient care experience only matters if you extract learning from it. Most healthcare providers waste their early clinical hours performing tasks without reflection, missing the patterns and insights that accelerate skill development. You need a deliberate approach to documentation and follow-up that transforms routine patient interactions into systematic education.
Start a detailed log of every significant patient encounter you observe or assist with. Record not just the presenting complaint but the clinical reasoning behind treatment decisions and the actual outcomes weeks or months later. Document specific procedures you performed, vital sign changes you noticed, and patient education moments where someone’s understanding shifted. This isn’t busywork-it’s the foundation for reflection.
After each shift, spend 15 minutes writing down one patient case that surprised you, one clinical decision you didn’t understand, and one moment where you saw how social factors affected care. Research answers to your own questions using evidence-based resources rather than waiting passively for someone to teach you. This active curiosity distinguishes providers who coast through clinical experience from those who genuinely develop judgment.
Seek Mentorship From Clinicians Who Value Teaching
Your mentor relationship determines whether your clinical experience compounds or stagnates. Seek out experienced clinicians in your setting who demonstrate the kind of practice you want to build-not necessarily the busiest or most prestigious person, but someone who clearly values patient relationships and invests time in teaching.
Ask directly if they’ll spend 15 minutes weekly discussing patient cases with you, and come prepared with specific questions about the patients you’ve encountered. Ask why they chose a particular medication over alternatives, how they identified that patient’s hidden social barrier, or what clinical sign made them suspect something serious. Request opportunities to observe them during patient education, medication counseling, or difficult conversations about treatment limitations.
The clinicians most willing to mentor work in settings where the pace allows for teaching moments. Direct Primary Care practices create the protected time needed for genuine mentorship relationships, removing the rushed environment that prevents experienced providers from investing in the next generation.
Track patient follow-ups to Understand Real Outcomes
Track your patient follow-ups obsessively-this separates meaningful learning from superficial exposure. When you discharge a patient from urgent care or assist with a new diabetes diagnosis in primary care, make a note to check on them two weeks later. Ask your supervising provider what happened with that patient’s lab work, whether the medication adjustment worked, whether they actually filled the prescription.
This continuity reveals what actually works in practice versus what looks good in theory. You’ll discover that the patient education you gave didn’t stick because you didn’t address their specific barrier to adherence, or that the treatment plan succeeded because your provider understood something about the patient’s life that changed the approach entirely. This feedback loop is what builds clinical judgment.
The patients you follow over time teach you lessons that isolated encounters cannot. You see which interventions produce lasting change and which ones fail silently after discharge. You learn that theory and practice diverge in predictable ways, and you develop the intuition to anticipate those gaps before they harm patients.
Final Thoughts
Direct patient care experience transforms how you practice medicine and shapes the clinical judgment that separates competent practitioners from exceptional ones. The hours you invest in meaningful patient interactions, the cases you follow from diagnosis through recovery, and the mentorship relationships you build create a foundation that no simulation or textbook can replicate. Providers who prioritize this experience develop better judgment, stronger patient relationships, and the practical skills that matter most in real clinical work.
The pathways to gain this experience remain diverse and accessible across entry-level clinical roles, community health centers, urgent care settings, and primary care environments. Each setting teaches something valuable about how patients actually experience healthcare, and the common thread connecting them all is your commitment to active learning and genuine engagement with the patients you serve. Whether you work as a medical assistant, volunteer in community health, or assist in urgent care, your deliberate reflection on patient outcomes accelerates your development far faster than passive observation ever could.
If you want a practice environment that prioritizes meaningful provider-patient relationships, Mosaic Medicine Clinic in Bradenton, Florida demonstrates what becomes possible when the healthcare model supports direct patient care experience. Start building your foundation today by seeking settings where you actively participate in patient care, finding mentors who value teaching, and committing to the reflection that transforms routine work into genuine learning.







