Your reproductive health shapes your quality of life at every stage. Yet many women receive fragmented care or miss preventative screenings that catch problems early.
At Mosaic Medicine Clinic, we believe female reproductive system health deserves a comprehensive approach-one that combines regular screening, early detection, and practical guidance tailored to your body’s needs. This guide walks you through what’s normal, what requires attention, and how to build a proactive partnership with your healthcare provider.
How Your Reproductive System Works
The Organs That Drive Your Cycle
Your reproductive system is a coordinated network of organs that regulate your menstrual cycle, produce hormones, and support fertility. Understanding how these pieces work together helps you recognize what’s normal for your body and spot warning signs early. The ovaries sit on either side of your uterus and perform two essential jobs: they release an egg each month during ovulation, and they produce estrogen and progesterone, the hormones that orchestrate your entire cycle.
The uterus itself is pear-shaped with thick muscular walls that thicken each month in preparation for pregnancy. If fertilization doesn’t happen, the lining sheds as your period. The fallopian tubes connect your ovaries to your uterus and are where fertilization typically occurs. Your cervix acts as a gateway between your uterus and vagina, and it changes throughout your cycle-the mucus thickens after ovulation to block sperm, but becomes stretchy and clear before ovulation to help sperm travel upward.
Reading Your Cervical Mucus
This shift in cervical mucus is one of the most reliable signs that ovulation is approaching. Tracking it gives you real insight into your fertile window without apps or expensive tests. The consistency changes from thick and opaque to egg-white and stretchy as estrogen rises, signaling peak fertility. Many women find this simple observation more informative than they expect.
The Four Phases of Your Cycle
Your menstrual cycle typically lasts about 28 days, though anywhere from 21 to 35 days is normal. The cycle has four distinct phases, and hormones orchestrate each one. During the follicular phase, your pituitary gland releases follicle-stimulating hormone, which tells your ovaries to grow eggs in fluid-filled sacs called follicles. Estrogen rises as the follicles develop, signaling your uterus to thicken its lining. One dominant follicle emerges while the others shrink and disappear.

Around day 14, a surge in luteinizing hormone triggers ovulation-the dominant follicle ruptures and releases the egg. After ovulation, the leftover follicle tissue becomes the corpus luteum and produces progesterone, which stabilizes your uterine lining and prepares it for implantation. This luteal phase lasts roughly 14 days and is more consistent than the follicular phase, which is why cycle length variation usually comes from differences in when you ovulate.
If no pregnancy occurs, progesterone and estrogen drop sharply, triggering menstruation. Normal variation matters here: some women ovulate on day 12, others on day 16, and both are completely healthy. Tracking your own patterns-whether through cervical mucus, basal body temperature, or simply noting when you bleed-reveals what normal looks like for you specifically.
Common Structural Variations
Structural variations are also common and usually harmless. Some women have a tilted uterus, others have a septate uterus with a wall running through the middle, and some have two separate uterine cavities. These differences rarely cause problems unless you’re trying to conceive or experiencing pain, in which case imaging during a gynecological exam can identify them. What matters most is understanding your own anatomy so you can communicate clearly with your healthcare provider about any symptoms or concerns.
Screening That Actually Catches Problems Early
Your annual gynecological exam forms the foundation of reproductive health care. During this visit, your provider performs a pelvic exam to check your ovaries, uterus, and cervix for abnormalities, discusses your menstrual patterns and any pain or bleeding changes, reviews your sexual history to assess STI risk, and screens for conditions like ovarian cysts or fibroids before they cause problems. This appointment also gives you space to ask about contraception options, fertility concerns, or hormonal symptoms that might signal thyroid issues or PCOS. Many women don’t realize that thyroid dysfunction directly affects your cycle-hypothyroidism can cause heavy periods and irregular ovulation, while hyperthyroidism can lighten your flow or stop it entirely.
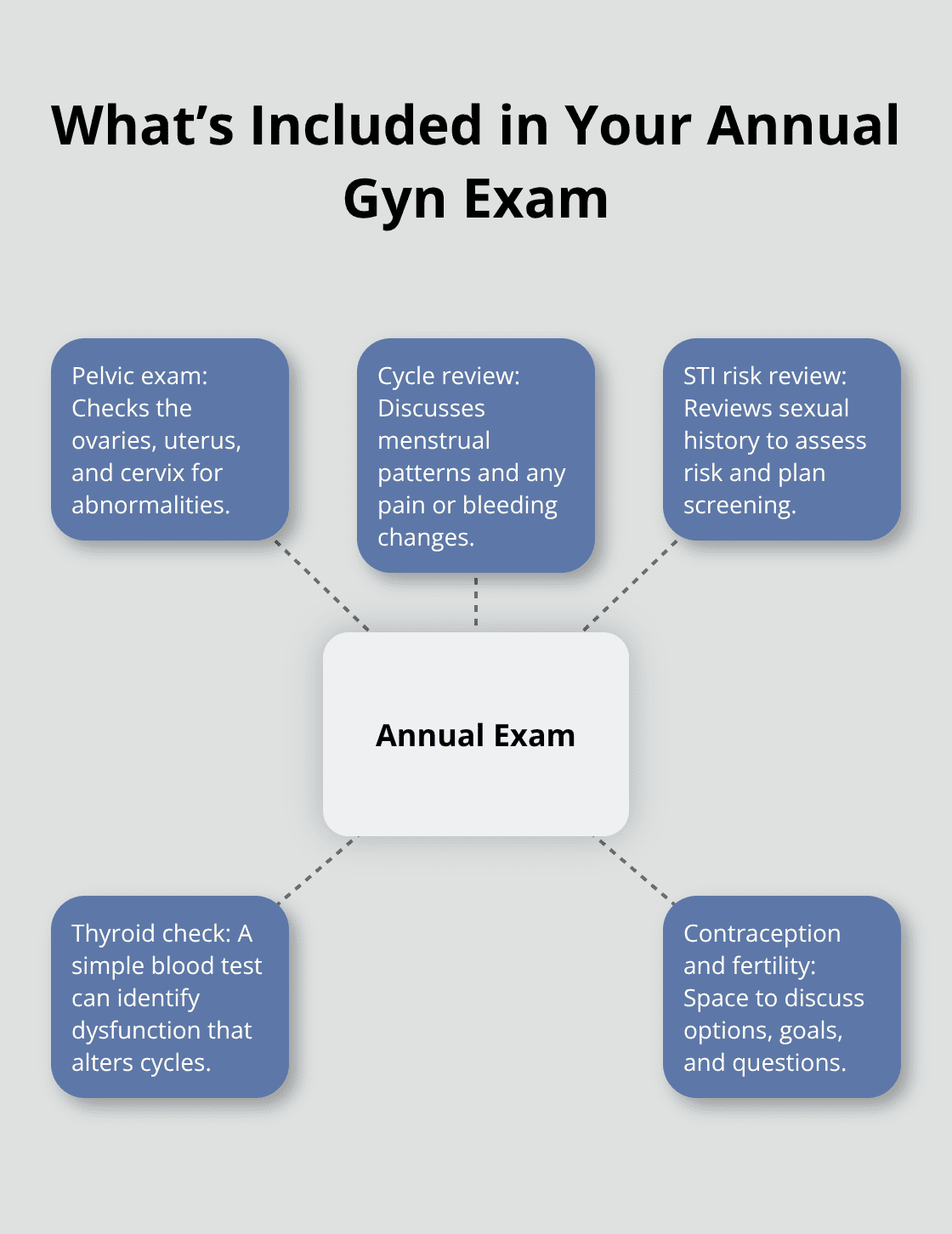
A simple blood test during your annual visit catches these issues early.
HPV Testing and Cervical Cancer Screening
Cervical cancer screening has become far more effective in recent years. The Women’s Preventive Services Initiative recommends cervical cytology every three years for women aged 21 to 29, and for women 30 to 65, either co-testing with HPV every five years or a Pap test alone every three years. HPV testing is the game-changer here-human papillomavirus causes nearly all cervical cancers, and knowing your HPV status guides how often you need screening. If you test negative for HPV, your risk of developing cervical cancer in the next 25 years drops to less than 1 percent, meaning you can space out screenings safely. This matters because it reduces unnecessary anxiety and over-screening while keeping you protected.
Bone Health in Midlife
Beyond reproductive screening, bone health deserves attention starting in midlife. Women lose bone density rapidly after menopause due to dropping estrogen levels, which increases fracture risk significantly. The Women’s Preventive Services Initiative recommends discussing bone health with your provider at midlife visits, particularly if you have risk factors like a family history of osteoporosis, low body weight, or limited physical activity. A DEXA scan measures bone density and guides whether you need preventative strategies like weight-bearing exercise, adequate calcium and vitamin D intake, or medication.
Cardiovascular Health and Risk Assessment
Cardiovascular disease is the leading cause of death for women in the United States, yet women often receive less aggressive prevention than men. Your annual exam should include blood pressure monitoring, lipid panel screening, and discussion of your personal and family cardiac risk. If you have multiple risk factors-smoking, obesity, diabetes, or a family history of early heart disease-your provider may recommend additional testing like an EKG or stress test before symptoms develop. Weight maintenance in midlife matters here too. The Women’s Preventive Services Initiative specifically recommends counseling women aged 40 to 60 with a normal BMI to maintain their weight through healthy eating and physical activity, since even modest weight gain in midlife increases cardiovascular and metabolic risk.
Building Consistency Into Your Care
These screenings work best when you maintain consistency. Schedule your annual visit at the same time each year, track your cycle length and any pain or bleeding changes, and be honest about your sexual history and lifestyle habits. This information gives your provider what they need to spot problems early and tailor recommendations to your specific health picture. With solid screening in place, you’re positioned to catch conditions before they progress-which brings us to the conditions that screening sometimes identifies and how to address them.
Common Conditions That Affect Reproductive Health
Endometriosis affects roughly 10 percent of reproductive-age women, yet diagnosis often takes years. Endometriosis causes inflammation, scar tissue, and pain that worsens during your period when tissue similar to your uterine lining grows outside the uterus. This delay happens because pelvic pain gets normalized or dismissed, and no simple blood test confirms the condition.
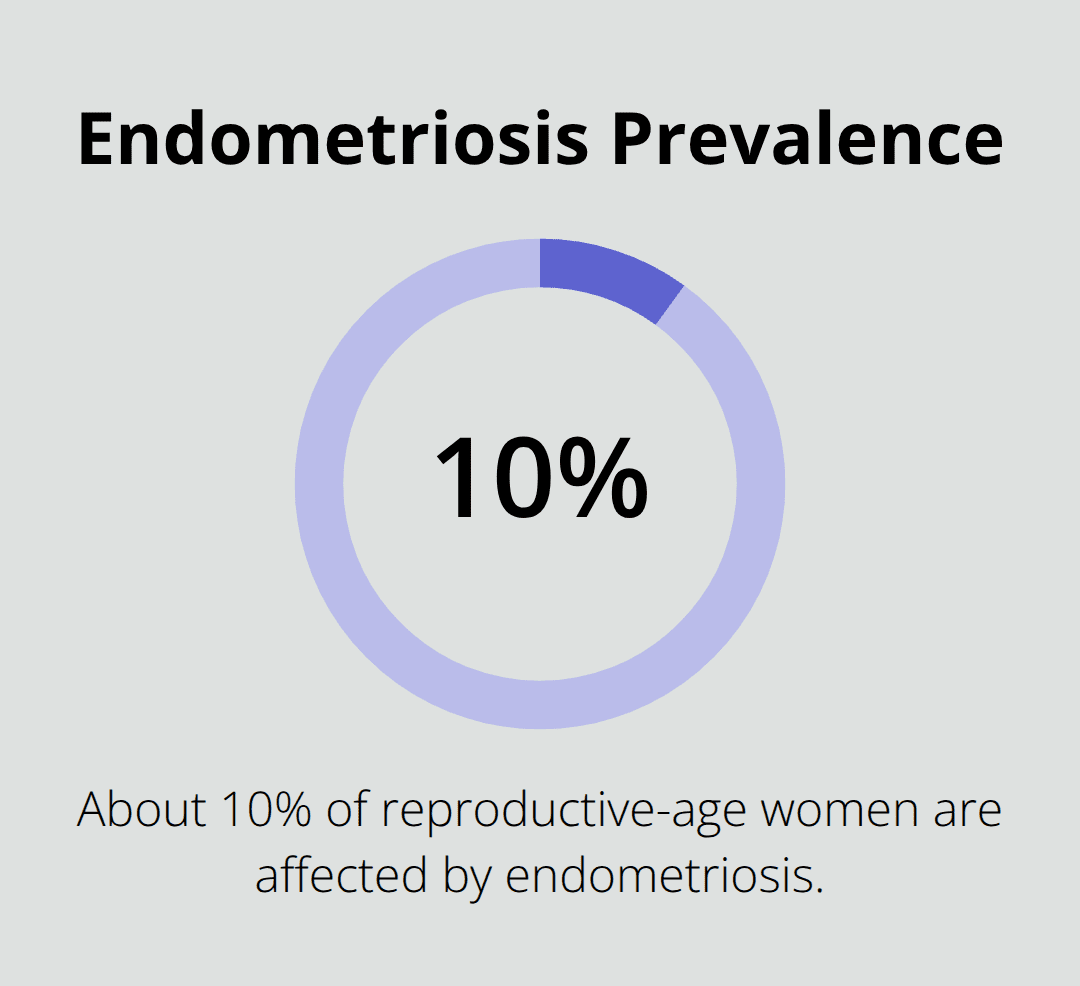
Endometriosis and Its Impact
Some women experience no symptoms at all-infertility becomes their first sign. If you have severe period pain that doesn’t respond to over-the-counter anti-inflammatories, pain during sex, or difficulty conceiving, imaging like ultrasound or MRI during your gynecological exam can identify endometrial lesions. Treatment ranges from hormonal contraceptives that suppress ovulation to surgical removal of affected tissue, depending on symptom severity and fertility goals.
PCOS: Hormones and Metabolic Risk
PCOS presents differently. It involves excess male hormones and multiple cysts on your ovaries, and the CDC notes that obesity increases risk significantly. Women with PCOS face higher rates of type 2 diabetes and heart disease, making early identification critical. Symptoms include irregular periods, infertility, excess facial or body hair, thinning scalp hair, acne, and dark patches of skin on your neck or armpits.
A pelvic ultrasound plus blood work measuring testosterone and other androgens confirms diagnosis. Management focuses on hormone balance-metformin often helps regulate your cycle and improve fertility, while weight loss through consistent exercise and dietary changes yields measurable improvements in hormone levels and ovulation.
Uterine Fibroids and Treatment Options
Uterine fibroids rank as the most common noncancerous uterine tumors in reproductive-age women, with African American women facing significantly higher risk. They cause heavy or prolonged periods, pelvic pain, frequent urination, pain during sex, and sometimes infertility or miscarriage. Ultrasound during your annual exam catches fibroids before symptoms escalate, and size and location determine treatment-some fibroids need monitoring only, while others require medication or surgical removal.
Infections That Demand Immediate Attention
Infections demand equally prompt attention. Sexually transmitted infections affect millions of women annually, and the CDC emphasizes that health consequences from STIs are often more severe for women than men. Some STIs like chlamydia and gonorrhea cause no symptoms initially, yet untreated infections progress to pelvic inflammatory disease, which damages your fallopian tubes and causes infertility. Bacterial and parasitic STIs respond to antibiotics, while viral STIs like herpes and HPV have no cure-antiviral medications manage symptoms, but prevention through vaccination and condom use matters more. Correct latex condom use greatly reduces but doesn’t eliminate STI transmission.
Bacterial vaginosis and yeast infections aren’t STIs but indicate an imbalance in your vaginal environment. Bacterial vaginosis involves an overgrowth of anaerobic bacteria and often causes gray or white discharge with a fishy odor. It increases your risk of pelvic inflammatory disease and pregnancy complications if left untreated, so mention any unusual discharge to your provider immediately.
Thyroid Dysfunction and Reproductive Health
Thyroid dysfunction directly impacts your reproductive health in ways many women miss. Hypothyroidism causes heavy periods, irregular cycles, and reduced fertility because inadequate thyroid hormone disrupts the communication between your brain and ovaries. Hyperthyroidism produces the opposite effect-lighter periods or amenorrhea. Your TSH level should be checked during your annual visit, especially if you experience cycle changes, fatigue, weight shifts, or difficulty conceiving. Thyroid medication restores normal ovulation and cycle regularity quickly once dosing stabilizes.
Final Thoughts
Your female reproductive system health depends on three things working together: knowing what’s normal for your body, staying consistent with screening, and speaking up when something feels off. Seek professional guidance if your periods become heavier or more painful than usual, your cycle shifts dramatically in length, you experience pain during sex, you notice unusual discharge, you struggle to conceive after a year of trying, or you develop symptoms like excess hair growth, fatigue, or unexplained weight changes. These aren’t minor complaints-they signal that something needs attention, and you deserve a provider who listens, investigates, and explains what’s happening.
Building a proactive healthcare partnership means finding a provider who takes time to understand your individual patterns and concerns. Schedule your annual exam, track what’s normal for you, and contact your healthcare team between visits when something changes. We at Mosaic Medicine Clinic focus on building strong relationships with our patients, offering direct access to physicians and comprehensive preventative medicine tailored to your needs.