Your mood swings might not be all in your head. Female hormones directly shape how your brain produces and uses chemicals that regulate emotions, anxiety, and mental clarity.
At Mosaic Medicine Clinic, we’ve seen firsthand how understanding the link between female hormones and mental health transforms how women manage their wellbeing. This guide walks you through what’s happening in your body and what you can actually do about it.
How Your Brain Chemistry Shifts With Your Hormones
Estrogen doesn’t just regulate your cycle-it directly controls how much serotonin your brain produces and uses. When estrogen rises during the follicular phase of your cycle, your brain synthesizes more serotonin, which improves mood, sharpens focus, and boosts motivation. Research from Harvard University shows that higher estrogen levels offer partial protection against emotional disturbance, while low estrogen during certain cycle phases increases vulnerability to mood disruption. The problem isn’t estrogen itself; it’s the withdrawal. When estrogen drops sharply before your period, serotonin production plummets, which explains why many women experience anxiety, sadness, and irritability in the week before menstruation.
About 60% of women with major depressive disorder report that their symptoms worsen during specific phases of their cycle, according to research published in The American Journal of Psychiatry. This isn’t coincidence-it’s biology. Progesterone amplifies this effect by stimulating calming neurotransmitters after ovulation, creating a window of relative emotional stability in the luteal phase.

But as both hormones fall approaching your period, that protective effect vanishes.
When Hormonal Shifts Become Severe
For about 5% of menstruating women, this hormonal shift triggers Premenstrual Dysphoric Disorder, or PMDD, which involves severe mood swings, anxiety, and depression that interfere with daily life. If you experience five or more emotional or physical symptoms in the week before your period that resolve when bleeding starts, PMDD may be the culprit. The distinction matters because PMDD responds well to specific treatments-SSRIs and certain birth control pills can significantly reduce symptoms when standard approaches fall short.
Why Timing Matters More Than You Think
The specific timing of hormonal changes determines whether you’ll experience mild mood shifts or significant mental health symptoms. A recent longitudinal study tracked women daily through their menstrual cycles and found that suicidal thoughts intensify just before menstruation, particularly in women with existing psychiatric conditions. This research, published in The American Journal of Psychiatry in 2023, emphasizes why clinicians need to ask detailed questions about your menstrual history during mental health evaluations.
If you’re already managing depression or anxiety, your cycle phase can dramatically amplify or reduce your symptoms. This means tracking isn’t optional-it’s essential. Apps or simple journals that record mood, anxiety levels, and cycle phase help you and your healthcare provider spot patterns that standard psychiatric assessments would miss.
Strategic Tools That Work With Your Biology
When your brain chemistry shifts predictably each month, you can prepare for vulnerable periods rather than being blindsided. Reducing caffeine and alcohol in the luteal phase, increasing aerobic exercise like walking or cycling, and prioritizing sleep become strategic moves rather than generic wellness advice. Research from 2022 shows that regular aerobic exercise significantly improves mood and energy during PMS and may reduce cramping, giving you a concrete tool that works with your hormones rather than against them. Understanding these patterns positions you to make informed decisions about your mental health care and recognize when professional support becomes necessary.
How Your Hormones Shift Across Life Stages
Your menstrual cycle isn’t the only time hormones reshape your mental health. Pregnancy, postpartum recovery, and menopause each bring distinct hormonal environments that directly alter brain chemistry and mood stability. Understanding what happens during these transitions helps you recognize when symptoms are hormonal versus when they signal something requiring immediate professional attention. Hormonal fluctuations create predictable patterns that differ significantly across these life stages, and what works during your cycle won’t necessarily work during perimenopause.
Pregnancy and the Postpartum Crash
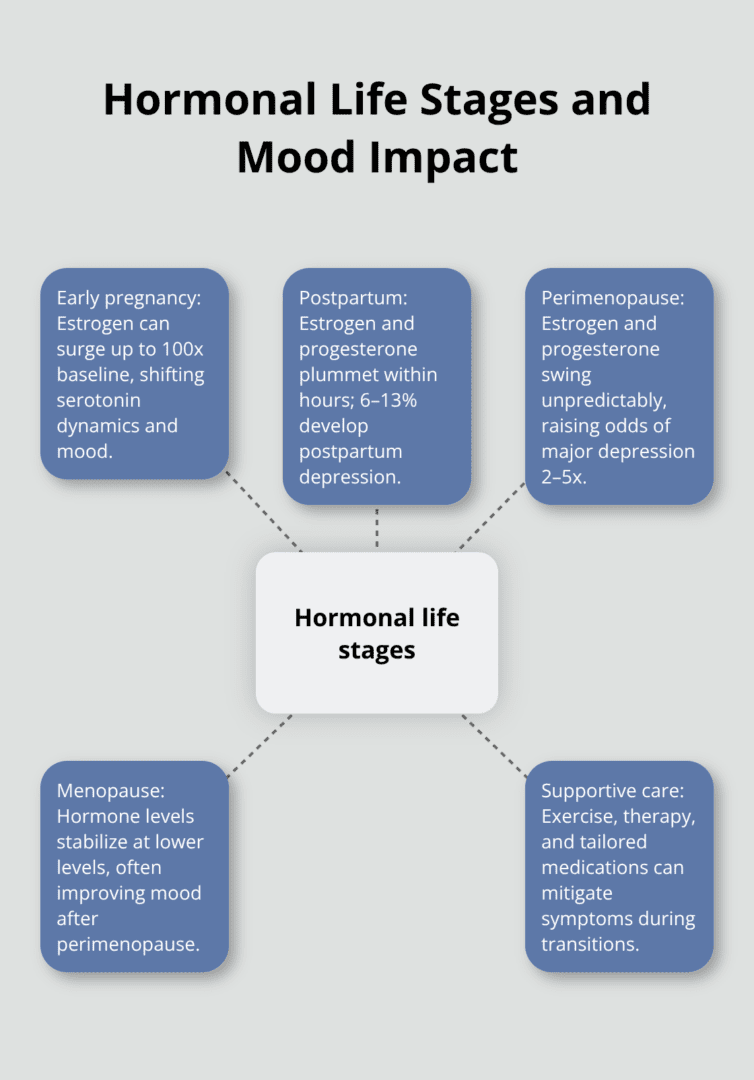
Estrogen during early pregnancy surges to levels up to 100 times higher than baseline, creating dramatic fluctuations in estrogen-serotonin dynamics that trigger mood changes, anxiety, and irritability in many women. Higher progesterone levels in the first trimester often bring fatigue and sadness alongside the physical symptoms you’re already managing. Most women experience mood improvement in the second trimester as hormone levels stabilize and energy increases.
The real danger emerges after birth. Within hours of delivery, estrogen and progesterone plummet dramatically, while endorphins provide only temporary relief. About 6 to 13 percent of new mothers develop postpartum depression, which is treatable but often goes unrecognized because people mistake it for typical new parent exhaustion.
If you experience persistent sadness, anxiety, difficulty bonding with your baby, or thoughts of harming yourself beyond the first two weeks after birth, that’s postpartum depression, not baby blues.
Sertraline, an SSRI antidepressant, shows documented improvement in remission rates compared to placebo for postpartum depression. Cognitive behavioral therapy and interpersonal therapy also work well, and breastfeeding itself can boost oxytocin and mood when it’s going smoothly. Social support matters enormously during this window-isolation amplifies postpartum mood disorders while consistent help from partners, family, or friends creates protective effects.
Perimenopause Brings the Steepest Hormonal Swings
Perimenopause represents the most extreme hormonal fluctuations you’ll experience outside of pregnancy. Your estrogen and progesterone levels don’t gradually decline; they swing wildly up and down across months and years before finally settling low. This erratic pattern creates 2 to 5 times higher odds of major depressive disorder during perimenopause compared to your reproductive years, according to research spanning multiple studies.
Women with a personal history of clinical depression face especially high risk of symptom recurrence during this transition. The mood changes can feel more severe than anything you experienced during your cycle because the hormonal swings are larger and more unpredictable. Menopause itself-defined as 12 consecutive months without menstruation-brings more stable hormone levels at the lower end, which paradoxically often improves mood once you’ve made it through the perimenopause chaos.
Tools That Work During Hormonal Transitions
Regular physical activity during this entire transition is associated with more positive mood and fewer depressive symptoms than low activity levels, making exercise one of your most concrete tools. Menopausal hormone therapy can relieve low mood for some women and help prevent depressive symptoms, but it carries cardiovascular and cancer risks that require careful discussion with your clinician to determine if it’s appropriate for your specific situation. If you’re taking antidepressants during perimenopause, pharmacogenetic testing can guide whether your current medication remains optimal as your hormones shift, potentially preventing the frustrating cycle of medication adjustments that many women experience during this decade.
These hormonal transitions reveal how deeply your reproductive biology shapes your mental health across your entire lifespan. The next section explores practical strategies you can implement right now to manage your mental health during these shifts, regardless of which life stage you’re navigating.
How to Track and Respond to Your Hormone-Mood Patterns
Tracking your cycle and mood isn’t optional busywork-it’s the foundation for managing your mental health effectively during hormonal transitions. Most women discover patterns only after months of daily records, which is why starting now matters more than waiting for the perfect tracking method. Apps like Clue or Flo let you log mood, anxiety levels, sleep quality, and cycle phase simultaneously, creating a visual map that reveals exactly when your symptoms peak. A study in The American Journal of Psychiatry found that suicidal ideation intensifies just before menstruation, particularly for those with existing psychiatric conditions-data that only emerges through consistent daily documentation, not monthly check-ins. Without this record, you and your healthcare provider operate on guesswork. With it, you can predict vulnerable periods three to four weeks in advance and adjust your strategies preemptively rather than reacting after symptoms hit. If apps feel overwhelming, a simple notebook works equally well; the format matters far less than consistency.

Document what time you take medications, when anxiety spikes, sleep hours, caffeine intake, and exercise-these variables interact with hormones in ways that standard psychiatric assessments miss entirely.
Identify Your Actual Vulnerabilities
Once you’ve tracked for two to three cycles, your actual vulnerabilities become obvious, and that’s when strategic lifestyle changes replace generic wellness advice. Reducing caffeine and alcohol during your luteal phase isn’t restriction; it’s protection, since these substances amplify anxiety when progesterone falls. Aerobic exercise shows documented improvements in mood during PMS, and the effect compounds when you time it intentionally-exercise more during vulnerable weeks rather than assuming consistency matters most. Eating protein-rich foods with complex carbohydrates boosts tryptophan absorption and serotonin production when estrogen dips; eggs, nuts, seeds, and legumes become functional tools rather than dietary recommendations.
Optimize Sleep and Nutrition
Sleep becomes non-negotiable during the luteal phase; limit caffeine after 2 pm and reduce blue light exposure before bed to prevent the sleep disruption that magnifies mood symptoms. Try foods rich in magnesium, omega-3 fatty acids, and B vitamins (leafy greens, legumes, fatty fish) to support brain function as hormones shift. These nutritional adjustments work with your biology rather than against it, creating measurable improvements within one to two cycles for many women.
Know When Professional Support Becomes Essential
If these adjustments don’t stabilize your symptoms within two cycles, or if you experience thoughts of self-harm, contact a mental health professional immediately rather than extending your self-care trial indefinitely. Pharmacogenetic testing can guide whether your current antidepressant remains optimal as your hormones shift, potentially preventing the frustrating medication shuffle many women endure. Direct access to your physician means you can discuss cycle-specific symptom patterns and medication adjustments without waiting weeks for appointments-that responsiveness transforms how quickly you can find relief when hormonal transitions destabilize your mental health.
Final Thoughts
Your hormones shape your mental health in measurable, predictable ways across every stage of your life. The connection between female hormones and mental health isn’t theoretical-it’s biology you can track, understand, and work with rather than against. When you recognize that mood swings, anxiety spikes, and depressive episodes often follow your hormonal patterns, you stop blaming yourself and start making informed decisions about your care.
The evidence is clear: estrogen withdrawal triggers mood disruption, progesterone creates windows of stability, and the hormonal transitions of pregnancy, perimenopause, and menopause reshape your mental health in ways that deserve professional attention. About 60% of women with depression report cycle-related symptom changes, and up to 5% experience PMDD severe enough to disrupt daily functioning. These aren’t rare experiences-they’re common patterns that respond to specific, evidence-based strategies.
Start tracking your cycle and mood today, even with a simple notebook. Within two to three cycles, you’ll see patterns that reveal exactly when you’re vulnerable and what actually helps. Adjust your caffeine, exercise, sleep, and nutrition strategically during high-risk phases rather than maintaining rigid consistency year-round. If symptoms persist despite these changes, or if you experience thoughts of self-harm, reach out to a mental health professional immediately, and consider how direct primary care can support your mental wellness through every hormonal transition.