Direct primary care has gained significant momentum across the United States, with over 1,300 practices now operating under this membership-based model. But is direct primary care working for the patients who choose it?
We at Mosaic Medicine Clinic see firsthand how this approach transforms healthcare relationships. The evidence shows compelling results in patient satisfaction, cost savings, and access to care.
Current State of Direct Primary Care Adoption
DPC Practices Multiply Across America
Direct primary care has expanded from a handful of practices to over 1,400 established clinics nationwide, representing growth of more than 1000% in just six years according to the American Medical Association. This expansion reflects a fundamental shift in how patients want to receive healthcare. The Medical Group Management Association found that 74% of healthcare leaders were unaware of the DPC model in 2018, but that awareness gap closes rapidly as more physicians and patients experience the benefits firsthand.
Patient Satisfaction Hits Record Levels
The numbers tell a compelling story about patient experience. Research shows that most respondents reported that DPC can offer positive experiences, with 85% of healthcare providers having heard of DPC according to recent studies. Patient retention rates in DPC practices consistently exceed 90% (indicating that once patients experience this model, they rarely return to traditional fee-for-service care). The Consumer Assessment of Healthcare Providers and Systems data reveals higher patient satisfaction scores across all metrics for DPC models compared to conventional practices.
Employers Drive Market Acceptance
Major employers take notice of DPC’s financial impact. Union County in North Carolina saved over $1.2 million in their first year with a DPC model for employee healthcare. Small businesses that use DPC report 54% fewer emergency room claims and 25% fewer hospital admissions compared to traditional models.
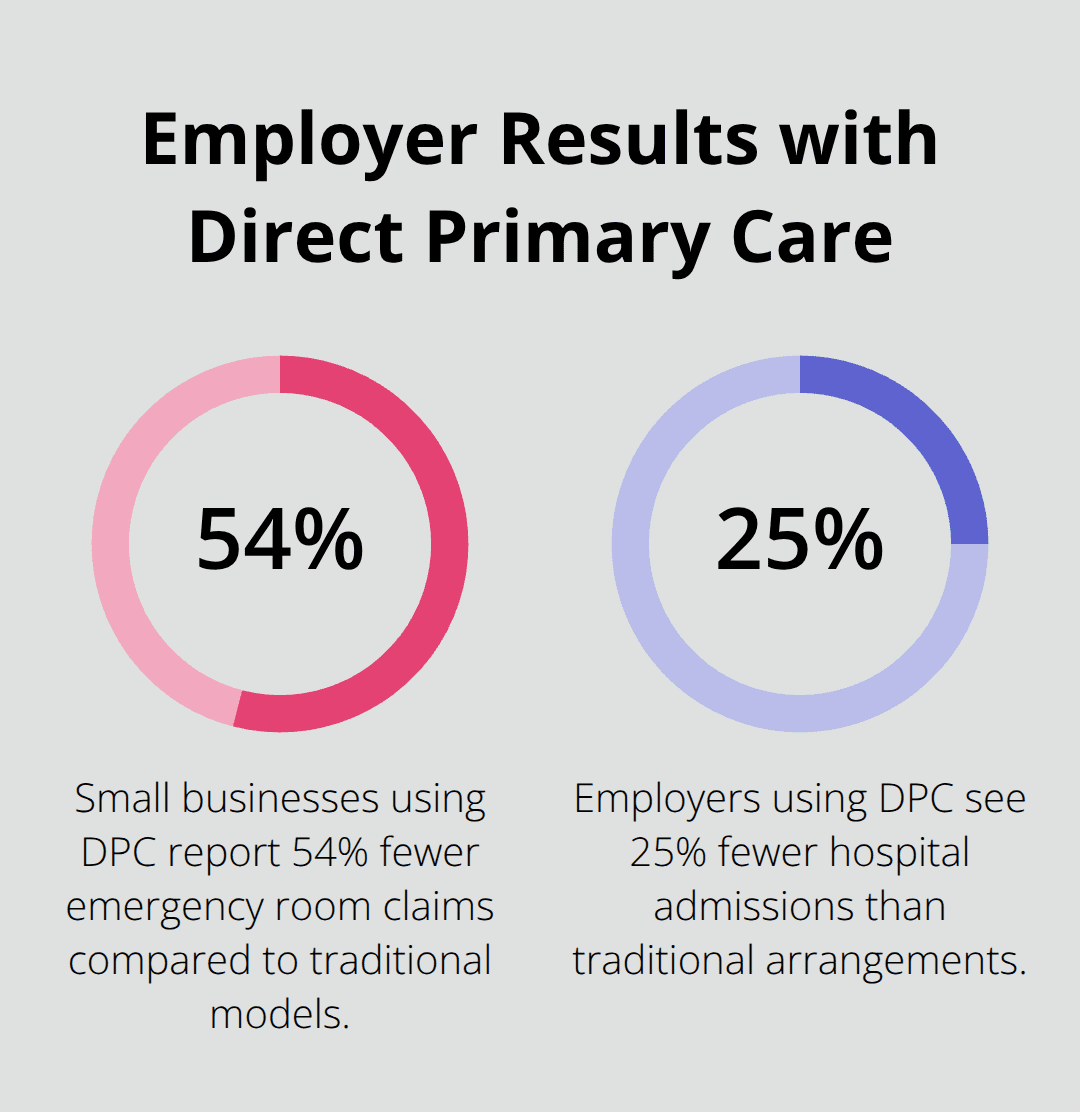
Traditional insurance companies initially viewed DPC as a threat, but many now recognize its potential to reduce overall healthcare costs (though the relationship remains complex as DPC practices operate outside traditional insurance frameworks).
These market shifts set the stage for examining how patients actually experience care under the DPC model.
Patient Outcomes and Experience with Direct Primary Care
Patient experience improves dramatically when administrative barriers disappear. Patients at DPC practices receive appointments within a few days compared to weeks in traditional settings, while DPC practices operate entirely outside the insurance system with patients paying monthly or annual fees directly to their physicians. The National Institutes of Health emphasizes that patient-reported experiences serve as key indicators of healthcare quality, and DPC patients consistently report better communication with their physicians. Text messages between patients and DPC clinicians have emerged as an effective tool for patient care, replacing phone trees and delayed callbacks that plague traditional practices.
Same-Day Access Becomes the Standard
Access to care transforms completely under the DPC model. Patients can schedule same-day or next-day appointments for urgent concerns, which eliminates the need for costly emergency room visits for non-emergency issues. DPC practices maintain smaller patient panels (typically 400-800 patients per physician compared to 2,500+ in traditional practices), which allows for immediate availability when patients need care most.
Transparent Costs Cut Healthcare Expenses
Cost transparency revolutionizes how patients approach healthcare decisions. DPC practices offer wholesale prices on labs and procedures, with patients who save 20-30% on healthcare costs when they combine DPC with high-deductible health plans. The average monthly membership fee of $77.38 replaces unpredictable copays and deductibles, while routine services like vaccines and basic procedures cost significantly less than traditional settings. Patients avoid the $2,300 average deductible of high-deductible health plans for primary care services.
Better Care Drives Improved Health Outcomes
Care access improves substantially in DPC settings. Only 8% of U.S. adults aged 35 and older received all recommended high-priority services in 2015, but DPC practices achieve higher rates through longer appointments and proactive outreach. Chronic disease management becomes more effective as physicians spend adequate time to address lifestyle factors, considering that nearly 80% of chronic conditions could be prevented through healthier lifestyle choices.
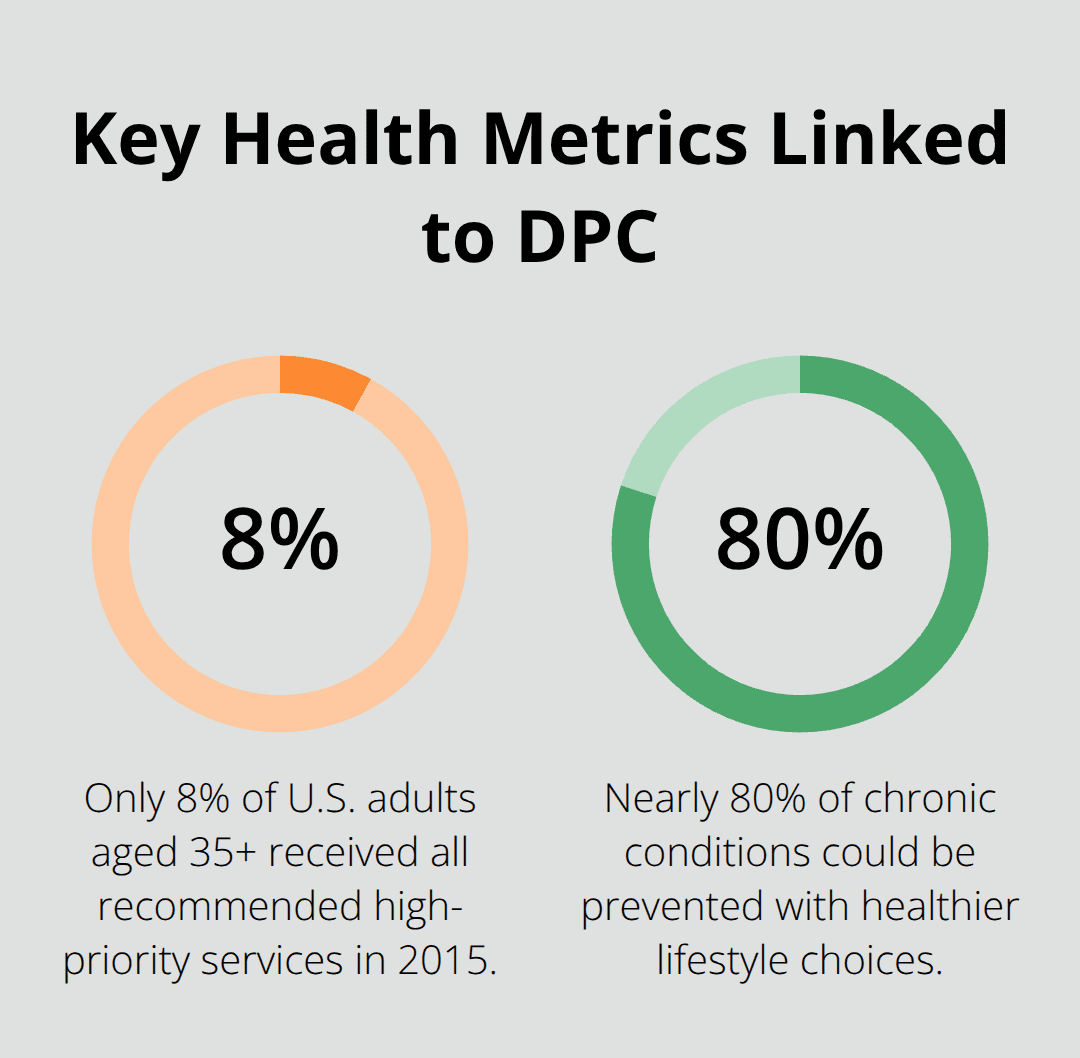
However, DPC practices face specific challenges that patients must consider before they make the switch to this model.
What Are DPC’s Biggest Weaknesses?
Direct primary care faces three significant limitations that patients must understand before they switch from traditional healthcare. Specialist referrals become more complex in DPC practices, as patients often encounter difficulties when they obtain timely appointments with specialists who may not accept DPC referrals directly. The lack of availability for brand-name medications creates ongoing challenges and forces DPC patients to pay high out-of-pocket costs for certain prescriptions that their monthly membership doesn’t cover.

Emergency services remain completely outside the DPC model and require patients to maintain separate insurance coverage or face substantial bills for hospital stays and emergency room visits.
Specialist Access Creates Real Barriers
Specialist care coordination proves problematic for many DPC patients. Traditional insurance networks facilitate specialist referrals through established relationships and pre-negotiated rates, but DPC practices operate outside these systems. Patients frequently wait longer for specialist appointments and pay higher costs without insurance negotiations. Some specialists refuse to see DPC patients altogether and limit treatment options for complex conditions that require ongoing specialist management.
Brand-Name Medications Cost More
Pharmaceutical access presents ongoing challenges for DPC patients who need specific brand-name medications. DPC practices typically offer generic medications at wholesale prices, but patients face high out-of-pocket costs when they require brand-name drugs that insurance formularies would normally cover. This limitation affects patients with chronic conditions who depend on specific medications that lack generic alternatives.
Insurance Requirements Still Apply
DPC practices cannot legally provide insurance coverage, which creates confusion among new patients who assume their monthly membership replaces all insurance needs. The American Medical Association’s Code of Medical Ethics requires clear disclosure that DPC memberships don’t constitute insurance, yet physicians who consider DPC switches report patient misunderstandings about coverage limitations. Emergency room visits, hospitalizations, and specialist care require separate insurance coverage (making DPC an addition to rather than replacement for traditional health insurance in most cases).
Final Thoughts
The evidence clearly shows that direct primary care works for patients who prioritize access, communication, and cost transparency. Patient satisfaction rates exceed 90%, appointment availability improves dramatically, and healthcare costs drop by 20-30% when combined with high-deductible plans. The 1000% growth in DPC practices over six years reflects genuine patient demand for this model.
Traditional healthcare models remain necessary for complex specialist care, emergency services, and patients who require extensive brand-name medications. DPC works best as part of a hybrid approach where patients maintain insurance for catastrophic coverage while they enjoy direct access to primary care. The question “is direct primary care working” receives a clear answer from the data and patient experiences.
The future points toward continued DPC expansion as more employers recognize the cost savings and patients experience the benefits of longer appointments and direct physician communication. DPC will likely complement rather than replace traditional models and offer patients choice in how they access primary care services. We at Mosaic Medicine Clinic believe this transformation creates stronger patient relationships and better health outcomes (though each patient must evaluate whether DPC fits their specific healthcare needs).
