Many patients feel confused when choosing between internal medicine and primary care physicians. Both provide essential healthcare services, but they serve different roles in your medical journey.
At Mosaic Medicine Clinic, we often help patients understand the internal medicine vs primary care distinction. This guide breaks down the key differences between these two medical specialties, helping you make informed decisions about your healthcare needs.
What Does Internal Medicine Actually Cover
Internal medicine physicians, known as internists, specialize exclusively in adult healthcare from age 18 onwards. These doctors complete four years of medical school followed by a three-year internal medicine residency program, then pass rigorous board certification exams administered by the American Board of Internal Medicine. Unlike family physicians who treat patients of all ages, internists dedicate their entire practice to adult diseases and conditions.
Adult-Focused Medical Training
The American College of Physicians reports that internists receive extensive training in hospital settings where they manage critically ill patients and complex medical cases. This intensive hospital experience sets them apart from other primary care providers. Internists train in subspecialties that include cardiology, endocrinology, gastroenterology, and infectious diseases (which gives them deep expertise in adult medical conditions). Many internists pursue additional fellowship training in areas like diabetes management or heart disease, which makes them highly specialized in chronic adult conditions.
Complex Disease Management
Internists excel at the management of multiple chronic conditions simultaneously, a common scenario as adults age. They routinely treat diabetes, hypertension, heart disease, chronic kidney disease, and autoimmune disorders. The Centers for Disease Control and Prevention data shows that 6 in 10 adults have at least one chronic disease, which makes internists particularly valuable for adult patients. These physicians coordinate care between multiple specialists, manage medication interactions, and create comprehensive treatment plans for patients with overlapping health issues.
Hospital and Outpatient Care
Internists work in both hospital and outpatient settings, which allows them to provide continuity of care across different healthcare environments. Their extensive hospital training prepares them to handle acute medical emergencies and manage transitions between inpatient and outpatient care effectively. This dual capability becomes particularly important when patients require hospitalization for chronic condition complications or develop new health problems that need immediate attention.
While internists focus specifically on adult medicine, primary care takes a broader approach to healthcare delivery across all age groups.
What Does Primary Care Include
Primary care serves as the foundation of healthcare delivery and provides comprehensive medical services to patients across all age groups and health conditions. The National Academy of Medicine defines primary care as first-contact, accessible, coordinated, and comprehensive healthcare that addresses the majority of personal health needs through sustained partnerships with patients. This broad approach distinguishes primary care from specialty medicine by focusing on whole-person care rather than single-organ systems or specific diseases.
The Four Types of Primary Care Providers
Family medicine physicians represent the largest group of primary care providers and complete three-year residencies that cover pediatrics, adult medicine, obstetrics, and basic surgical procedures. The American Academy of Family Physicians reports that family doctors provide care for patients from birth through end of life, which makes them ideal for families who want one provider for all members. Pediatricians focus exclusively on children from birth to age 18 and complete three-year residencies in child development, growth patterns, and childhood diseases.

Internal medicine physicians serve as primary care providers for adults only, while nurse practitioners and physician assistants increasingly fill primary care roles after they complete specialized programs that range from 24 to 36 months.
Comprehensive Service Range in Primary Care Settings
Primary care practices offer preventive services that include annual physicals, immunizations, cancer screenings, and health risk assessments. Preventive care helps reduce healthcare costs and improves patient outcomes when patients maintain regular primary care relationships. These providers manage acute conditions like infections, injuries, and sudden illness episodes while they coordinate chronic disease management for conditions such as diabetes, hypertension, and asthma. Primary care physicians also provide mental health screenings, basic counseling services, and referrals to specialists when complex conditions require focused expertise beyond their scope of practice.
The distinction between internal medicine and primary care becomes clearer when you examine the specific patient populations each specialty serves and how their practice approaches differ fundamentally.
How Do These Specialties Differ in Practice
Age Groups and Patient Populations
The most significant difference lies in patient demographics. Internal medicine physicians exclusively treat adults aged 18 and older, while primary care encompasses all ages from newborns to elderly patients. The American Academy of Family Physicians data shows that family medicine doctors treat an average of 2,300 patients annually across all age groups, whereas internists typically manage 1,800 to 2,000 adult patients. This age restriction allows internists to develop deeper expertise in adult-specific conditions like cardiovascular disease, diabetes complications, and age-related hormonal changes.
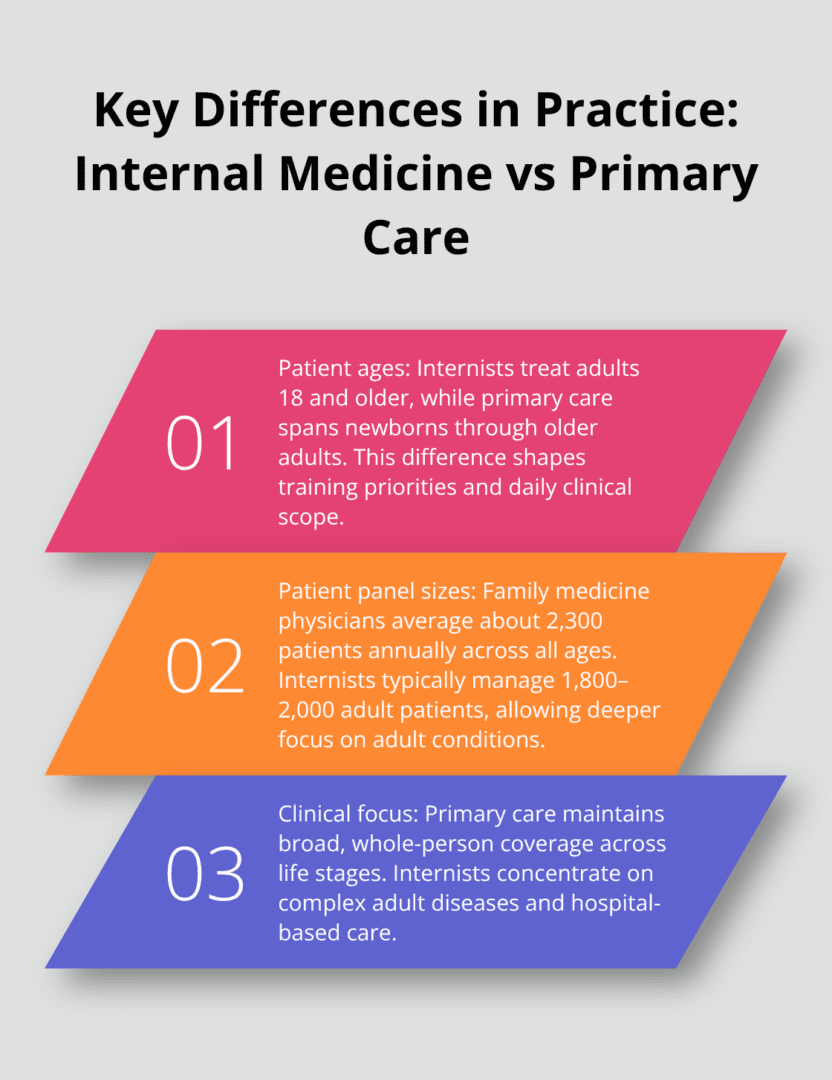

Primary care providers must maintain knowledge across pediatric vaccines, childhood development, adult preventive care, and geriatric medicine simultaneously.
Specialty Focus and Practice Depth
Internists concentrate exclusively on adult diseases and often subspecialize further. The American Board of Internal Medicine recognizes 19 subspecialties that include cardiology, endocrinology, and rheumatology. Many internists pursue additional fellowship training after residency, which creates highly specialized adult medicine experts. Primary care providers maintain broader knowledge across multiple medical areas but with less depth in specific adult conditions. Family physicians spend significant training time on obstetrics, pediatrics, and basic procedures, while internists dedicate their entire education to complex adult medical conditions and hospital-based care.
Care Coordination Approaches
Internists typically coordinate care among multiple adult medicine specialists and manage complex medication regimens for patients with overlapping chronic conditions. They often serve as the central hub for patients who see cardiologists, endocrinologists, and other adult specialists. Primary care providers coordinate across a wider range of specialists that include pediatricians, obstetricians, orthopedists, and mental health professionals depending on their patient population. The coordination complexity differs significantly when primary care providers manage entire families with diverse medical needs versus internists who focus solely on adult specialty referrals and chronic disease management. Finding the right healthcare provider requires understanding these fundamental differences in practice approaches.
Final Thoughts
The internal medicine vs primary care decision depends on your specific health needs and family situation. Internal medicine physicians offer specialized adult-focused care with deep expertise in complex chronic conditions, while primary care providers deliver comprehensive healthcare across all ages with broader medical knowledge. Adults with multiple chronic conditions like diabetes, heart disease, or autoimmune disorders often benefit from an internist’s specialised training and hospital experience.
Families with children typically prefer primary care providers who can treat all family members and coordinate diverse medical needs under one roof. Consider your current health status, family composition, and preference for specialist versus generalist care when you make this choice. Patients in good health may thrive with either option, while those who manage complex medical conditions might prefer the focused expertise that internists provide.
We at Mosaic Medicine Clinic bridge traditional healthcare gaps through our Direct Primary Care model. Our membership-based approach provides unrushed appointments, direct physician access, and transparent pricing (with wholesale labs and discounted medications). We focus on building strong patient-doctor relationships while we make quality healthcare more accessible and affordable for individuals, families, and small businesses. Learn more about our innovative approach to personalized healthcare delivery.











